Key Takeaways
-
1System Beats Survey: A one-time survey collects data, while a patient feedback system creates a continuous loop that turns insights into measurable operational and clinical improvements.
-
2Act on Feedback: Collecting feedback without following up damages trust. Patients who see their input produce visible changes are more likely to return and refer others.
-
3Use Multiple Channels: Combining SMS surveys, in-clinic kiosks, patient portal feedback, and online review monitoring ensures data represents the full patient population.
-
4Train Your Staff: Even advanced feedback tools fail if front-desk and clinical teams are not trained to collect, escalate, and act on feedback consistently.
-
5Feedback as Intelligence: Beyond satisfaction scores, feedback systems reveal scheduling bottlenecks, communication gaps, staffing issues, and workflow problems faster and more accurately than internal audits.
Did you know? Patient feedback is your clinic’s secret weapon. What if one simple system could reveal exactly what your patients love and what’s driving them away?
Implementing a smart patient feedback system can change your clinic’s care, boost satisfaction, and turn every visit into an opportunity for growth.
In the modern healthcare environment, patients expect more than competent clinical care. They want a seamless, personalized experience, from appointment booking to post-visit follow-up.
Increasingly, patients evaluate clinics not only on treatment outcomes but also on factors like staff communication, wait times, ease of scheduling, and the overall sense of care coordination.
Rising expectations, especially around digital engagement, transparency, and convenience, make understanding patient perspectives more important than ever.
A patient feedback system provides a structured, actionable framework for capturing patient insights, analyzing them, and making meaningful improvements.
Unlike one-off surveys, it establishes a continuous healthcare feedback loop, allowing clinics to identify recurring issues, optimize workflows, and strengthen the patient-provider relationship.
Implementing an effective feedback system does more than collect opinions, it transforms patient insights into strategies for enhancing care quality, operational efficiency, and patient satisfaction.
Clinics that embrace patient feedback systematically often see:
- Improved patient retention and loyalty.
- Reduced missed appointments and cancellations.
- Better staff performance through targeted training.
- Enhanced online reputation and community trust.
The goal is to go beyond simply gathering feedback, clinics must act on it. Listening to patients is important, but following through is what drives real improvements in patient care improvement and clinic operations.
Table of Contents
What a Patient Feedback System Really Is
A patient feedback system is a structured process designed to capture, analyze, and apply patient insights consistently. It ensures that feedback is not just collected, but also translated into actionable steps that improve care delivery and operational performance.
For example: Consider a clinic noticing multiple patients reporting frustration with long wait times. Through a structured system, the clinic can not only identify this issue but also implement workflow adjustments, train staff to improve scheduling, and monitor outcomes over time. This demonstrates how feedback directly impacts care quality and operational efficiency.
Feedback can be gathered through various channels:
- Digital platforms: Patient portals, mobile apps, and post-visit emails allow real-time patient feedback. These platforms provide instant access to patient opinions, which can be aggregated and analyzed for trends.
- In-clinic methods: Kiosks, paper forms, or suggestion boxes capture input from patients who prefer traditional methods. Immediate feedback can help staff address concerns on the spot, improving patient satisfaction.
A key difference between a feedback system and a single survey is the continuous nature of the process. Clinics can monitor patterns over time, identify emerging issues, and evaluate the impact of changes.
By establishing a healthcare feedback loop, clinics ensure patient voices are integrated into ongoing improvements, enhancing both the patient experience and operational efficiency.
Why Patient Feedback Matters for Clinics

Patient feedback is critical for clinics seeking to improve service quality, patient experience, and operational efficiency. Here’s why:
- Identify areas for improvement: Feedback helps clinics spot problems before they escalate. For instance, recurring complaints about unclear instructions may indicate the need for improved patient communication protocols.
- Strengthen patient relationships: Patients who feel heard are more likely to stay with the clinic long-term, fostering loyalty and improving the patient-provider relationship.
- Reduce missed appointments: Dissatisfied patients are more likely to skip appointments. Feedback allows clinics to proactively address concerns, reducing cancellations and no-shows.
- Support operational efficiency: Insights from feedback can uncover bottlenecks in scheduling, staffing, or administrative workflows, allowing the clinic to allocate resources more effectively.
- Enhance reputation: Patients who see their feedback acted upon are more likely to leave positive reviews online, strengthening the clinic’s public image.
Example: A mid-sized clinic implemented a structured feedback system and discovered that patients frequently canceled appointments due to unclear pre-visit instructions.
Multiple surveys show that patients pay close attention to how clinics handle feedback: more than 80% of patients read online reviews when choosing a provider, and nearly 60% say they trust providers more when they see them responding to reviews and addressing concerns.
In other words, acting on feedback doesn’t just improve experience scores—it directly influences whether patients stay, return, and recommend the practice to others.
Types of Patient Feedback You Can Collect
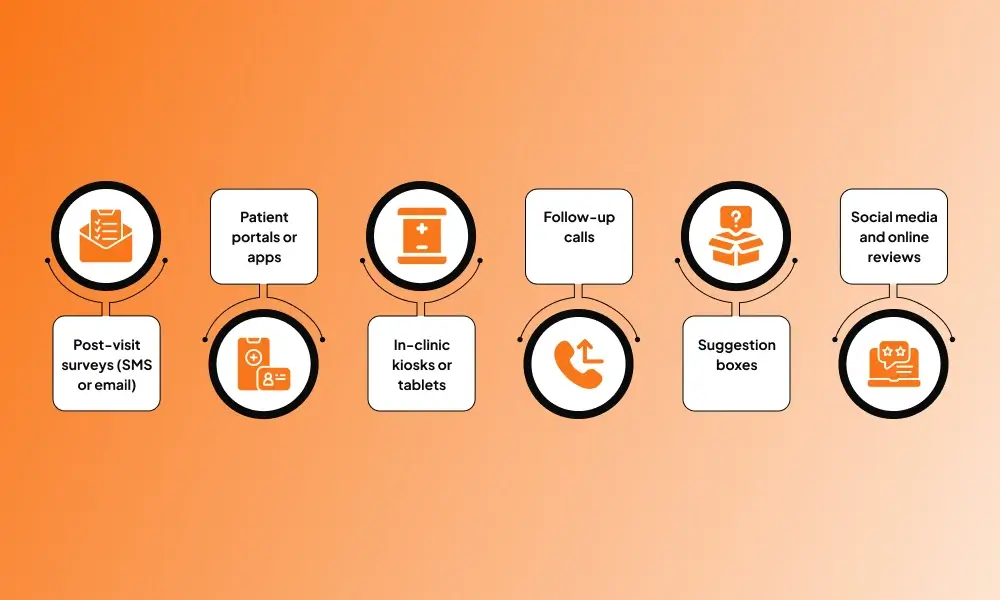
Feedback should be collected through multiple channels to provide a comprehensive understanding of patient experiences. Each method has advantages and challenges:
- Post-visit surveys (SMS or email): Ideal for quick feedback on a recent visit. Pros: easy to implement, immediate responses. Cons: low response rates if surveys are too long.
- Patient portals or apps: Digital platforms support ongoing feedback and patient sentiment analysis. Pros: convenient, integrated with clinic systems. Cons: requires tech adoption by patients.
- In-clinic kiosks or tablets: Capture immediate impressions during check-out. Pros: real-time data, high engagement. Cons: limited to in-person visits.
- Follow-up calls: Personalized conversations provide qualitative insights. Pros: detailed feedback, builds relationships. Cons: time-intensive for staff.
- Suggestion boxes: Capture unstructured ideas or concerns. Pros: freeform feedback, patient creativity. Cons: may require manual analysis.
- Social media and online reviews: Offer insights into public perception and overall reputation. Pros: wide reach, immediate visibility. Cons: not always actionable.
Combining multiple feedback channels ensures the data collected is representative and actionable. It also allows clinics to identify trends across different touchpoints, helping to improve overall patient satisfaction and clinic operations.
Step-by-Step Guide for an Effective Patient Feedback System

Step 1: Define Clear Goals
A patient feedback system without clearly defined goals produces data that no one knows how to act on. Before selecting a single tool or sending a single survey, every clinic needs to establish exactly what it is trying to learn, improve, and measure.
Those goals need to be specific enough to drive decisions rather than so broad that they could describe any healthcare organization. Clear objectives ensure the feedback collected leads to meaningful improvements in patient experience and practice operations.
Generic goals like “improve patient satisfaction” or “collect more feedback” are not true goals, they are wishes. An effective operational goal is specific, such as reducing the percentage of patients reporting wait times over 20 minutes from 34 percent to under 15 percent within 90 days. This clearly defines what to measure, which tools to use, the target threshold, and when to evaluate results.
How to define feedback goals that actually drive improvement:
- Audit your current patient complaints first — before setting goals, review the last 90 days of complaints, negative online reviews, cancellation reasons, and no-show patterns to identify where patient dissatisfaction is already surfacing; your feedback goals should address the problems you already know exist before attempting to discover new ones
- Align goals with operational priorities — if your practice is focused on reducing no-shows, your feedback goals should measure scheduling experience, reminder effectiveness, and appointment confirmation satisfaction; if your priority is growing referrals, your goals should measure net promoter score and likelihood to recommend
- Set goals at three levels — practice-wide goals that apply to all locations and providers, department-level goals that address specific workflow areas such as front-desk communication or provider explanation clarity, and individual provider goals that support performance reviews and targeted coaching
- Make every goal time-bound and measurable — attach a specific metric, a baseline value, a target value, and a review date to every goal so progress can be evaluated objectively; open-ended goals with no measurement criteria cannot be meaningfully tracked or improved
- Involve clinical and administrative leadership in goal-setting — feedback goals that are set by one department and handed to another without buy-in produce resistance rather than improvement; bring together providers, front-desk managers, billing staff, and care coordinators to agree on which feedback priorities matter most to the practice as a whole
- Review and update goals quarterly — patient needs, operational priorities, and competitive pressures change; a feedback goal that was urgent six months ago may be resolved while a new priority has emerged; static goals that are never revisited produce static improvement
Examples of strong patient feedback goals by priority area:
| Priority Area | Weak Goal | Strong Goal |
|---|---|---|
| Wait times | Reduce wait times | Reduce the percentage of patients rating wait time as poor from 28% to under 10% within 60 days |
| Provider communication | Improve communication scores | Increase provider explanation clarity rating from 3.6 to 4.2 out of 5 within 90 days |
| Scheduling experience | Make scheduling easier | Reduce scheduling friction complaints by 40% within 45 days of implementing online booking |
| Staff friendliness | Improve staff attitude | Achieve a front-desk friendliness score above 4.5 out of 5 across all locations within 60 days |
| Net Promoter Score | Get more referrals | Increase NPS from 32 to 50 within 6 months by improving post-visit follow-up communication |
Step 2: Choose the Right Tools & Technology
The tools you choose determine whether your feedback system runs automatically in the background or requires constant manual effort to maintain. Most clinics that abandon their feedback systems do so not because they lost interest in patient feedback but because they chose tools that created more work than they eliminated.
The right patient feedback technology for your clinic depends on four factors: your patient volume, your existing EHR and scheduling infrastructure, your staff’s technical comfort level, and the specific feedback channels your patient population actually uses.
A tool that works brilliantly for a 10-provider multi-location group practice will be unnecessarily complex and expensive for a single-provider primary care clinic — and vice versa.
What to evaluate when choosing patient feedback tools:
- EHR and scheduling system integration — the single most important evaluation criterion; a feedback tool that does not integrate with your EHR requires manual data entry, creates duplicate records, and will be abandoned within weeks; confirm that any tool you evaluate has a native integration or a verified API connection with your specific EHR platform before investing
- Automation capability — the tool should be able to trigger survey delivery automatically based on visit completion, appointment type, or diagnosis without requiring a staff member to manually send each survey; manual feedback distribution is not scalable and produces inconsistent data
- Multi-channel delivery — patients have different communication preferences; your feedback tool must support SMS, email, patient portal messaging, and in-clinic tablet collection as minimum channels so you can reach patients through the channel they actually use rather than the one that is easiest for your staff
- Response rate optimization features — look for tools that support personalized survey invitations, configurable send timing, automated reminders for non-responders, and survey length optimization; these features have a direct measurable impact on response rates and data quality
- Real-time dashboard and reporting — feedback data that requires a manual export and analysis every month does not get reviewed or acted on; choose a tool with a live dashboard that displays satisfaction trends, response rates, and alert flags for negative feedback in real time so issues are identified and addressed within hours not weeks
- Negative feedback alerting — the tool should automatically flag responses below a defined satisfaction threshold and route them to the appropriate manager or care coordinator for same-day follow-up; automated negative feedback alerts are the most direct path from feedback collection to patient retention
- HIPAA compliance — any tool that collects, stores, or transmits patient feedback is handling protected health information and must be fully HIPAA compliant with a signed Business Associate Agreement; verify compliance documentation before purchasing and never use general consumer survey tools like Google Forms or SurveyMonkey without confirming their BAA availability
- Scalability — choose a tool that can grow with your practice; a platform that handles 500 monthly surveys efficiently may perform poorly at 5,000; confirm pricing structure and performance benchmarks at your anticipated volume before committing
Tool categories to evaluate by use case:
| Tool Category | Best For | Key Limitation |
|---|---|---|
| EHR-integrated feedback modules | Practices wanting minimal vendor complexity | Limited customization and channel flexibility |
| Dedicated patient experience platforms | Multi-location groups needing advanced analytics | Higher cost, longer implementation timeline |
| SMS-first survey tools | High response rate priority, mobile-heavy patient population | Limited qualitative data collection |
| In-clinic kiosk systems | High walk-in volume, elderly or less tech-savvy patients | No between-visit or post-visit data capture |
| Patient portal survey features | Practices with high portal adoption rates | Low engagement from patients who rarely use the portal |
Step 3: Decide What to Measure
Measuring everything produces insight about nothing. The most common reason patient feedback data sits unused in a dashboard is that the clinic collected 40 different metrics across every possible touchpoint and has no framework for deciding which numbers to prioritize, which to ignore, and which to escalate.
Effective patient feedback measurement starts with choosing a focused set of metrics that are directly connected to your operational goals, are actionable when they move in either direction, and can be tracked consistently over time against a defined baseline.
Core metrics every clinic should measure:
- Patient Satisfaction Score (CSAT) — measures overall satisfaction with a specific visit or interaction on a numeric scale; typically collected immediately after the visit when experience recall is highest; the most common baseline metric for tracking improvement over time
- Net Promoter Score (NPS) — measures patient likelihood to recommend your practice to friends or family on a 0 to 10 scale; NPS above 50 is considered strong for healthcare; NPS below 30 signals retention and referral risk that requires immediate investigation
- Wait time satisfaction — measures patient perception of wait time at scheduling, check-in, and in the exam room separately; perceived wait time consistently drives satisfaction scores more than actual wait time, making this one of the highest-leverage metrics to track and improve
- Provider communication score — measures how clearly the provider explained the diagnosis, treatment options, and next steps; low scores here are strongly correlated with poor care plan adherence, increased patient complaints, and higher no-show rates at follow-up appointments
- Scheduling and access satisfaction — measures how easy patients found it to book an appointment, reach the practice by phone, and access same-day or urgent care when needed; scheduling friction is one of the top three reasons patients leave a practice
- Staff friendliness and professionalism — measures patient perception of front-desk, nursing, and administrative staff interactions; staff attitude scores that vary significantly between locations or providers in a group practice indicate a training or culture gap that requires targeted intervention
- First contact resolution rate — measures the percentage of patient concerns resolved in a single interaction without requiring callbacks, escalations, or repeat contacts; low first contact resolution rates indicate communication inefficiency that frustrates patients and consumes staff time simultaneously
Benchmarks to target by metric:
| Metric | Needs Improvement | Acceptable | Strong Performance |
|---|---|---|---|
| Overall CSAT | Below 80% | 80–89% | 90% and above |
| Net Promoter Score | Below 30 | 30–50 | Above 50 |
| Wait time satisfaction | Below 70% positive | 70–84% positive | 85% and above positive |
| Provider communication | Below 4.0 out of 5 | 4.0–4.4 out of 5 | 4.5 and above out of 5 |
| Survey response rate | Below 15% | 15–30% | Above 30% |
| Negative feedback escalation | Unresolved within 72 hours | Resolved within 48 hours | Resolved within 24 hours |
What not to measure:
Avoid measuring too many metrics simultaneously in the early stages — start with 3 to 5 core metrics, establish baselines, and add additional metrics only after your team has developed the capacity to review and respond to data consistently
Avoid tracking metrics you cannot act on operationally — if your clinic cannot change the physical facility layout, measuring facility appearance satisfaction as a priority metric produces frustration not improvement
Step 4: Design Patient-Friendly Surveys
Survey design is where most patient feedback systems quietly fail. A survey that is too long gets abandoned halfway through. A survey that uses clinical terminology confuses patients and produces inaccurate responses.
A survey that asks leading questions produces data that feels positive but reveals nothing actionable. A survey sent three days after the visit asks patients to recall details they have already forgotten.
The goal of patient survey design is to make completion feel effortless while producing data that is specific enough to drive operational decisions.
Core principles of effective patient survey design:
- Keep surveys under 5 questions for post-visit collection — research across healthcare survey platforms consistently shows that completion rates drop sharply beyond 5 questions for post-visit SMS and email surveys; if you need more comprehensive data, use a two-tier approach where a short 3-question survey goes to all patients and a longer optional survey is offered to patients who indicate willingness to provide more detailed feedback
- Send within 2 to 4 hours of visit completion — patient recall of specific interaction details degrades rapidly after leaving the clinic; surveys sent within 2 to 4 hours of visit completion consistently produce higher response rates and more accurate, specific feedback than surveys sent 24 or 48 hours later
- Open with the easiest question — begin every survey with a simple overall satisfaction rating question before asking for specific feedback; patients who commit to answering the first question are significantly more likely to complete the remaining questions than patients who encounter a complex or detailed question first
- Use plain language throughout — write every survey question at a sixth grade reading level; avoid clinical terminology, double negatives, and compound questions that ask about two things simultaneously; a question like “Was our staff communicative and professional?” cannot be answered accurately because a patient may rate communication positively and professionalism negatively
- Include at least one open-ended question — quantitative scores tell you how much patients are satisfied or dissatisfied; open-ended questions tell you why; include one optional open-ended question such as “Is there anything we could have done better during your visit today?” at the end of every survey to capture qualitative context that numeric scores cannot provide
- Personalize the survey invitation — address patients by first name in the survey invitation message, reference the specific visit type or provider they saw, and explain in one sentence why their feedback matters; personalized invitations consistently outperform generic invitations in both open rates and completion rates
- Make the thank-you message meaningful — close every survey with a genuine thank-you that confirms the feedback will be reviewed and acted on; patients who believe their feedback is read are more likely to complete future surveys; patients who feel their input disappears into a void stop participating
Survey question examples by measurement area:
| Measurement Area | Example Question | Response Format |
|---|---|---|
| Overall satisfaction | How would you rate your overall experience during today’s visit? | 1–5 star rating |
| Wait time | How satisfied were you with your wait time today? | Very satisfied / Satisfied / Neutral / Dissatisfied / Very dissatisfied |
| Provider communication | How clearly did your provider explain your diagnosis and next steps? | 1–5 scale |
| Staff friendliness | How would you rate the friendliness and professionalism of our staff? | 1–5 scale |
| Net Promoter Score | How likely are you to recommend our practice to a friend or family member? | 0–10 scale |
| Open feedback | Is there anything we could have done better today? | Open text field |
Step 5: Integrate Feedback Into Daily Workflows
A patient feedback system that exists separately from clinic operations is often ignored. Sustainable systems are embedded into daily workflows like scheduling, check-out, staff huddles, and care coordination so feedback is collected and acted on automatically.
How to embed feedback into workflows:
- Trigger surveys automatically — Configure your tool to send a survey when a visit is marked complete in your EHR or scheduling system so no patients are missed.
- Add verbal prompts at check-out — Train front-desk staff to tell patients, “You will receive a short survey by text — your feedback helps us improve.”
- Assign daily review roles — Designate a staff member to review the previous day’s feedback each morning so issues can be addressed promptly.
- Discuss trends in team huddles — Spend 2–3 minutes reviewing negative feedback, recurring patterns, and same-day concerns to keep the team informed.
- Route alerts immediately — Configure automatic alerts to the relevant manager, care coordinator, or provider when responses fall below satisfaction thresholds.
- Use feedback to adjust scheduling — Identify times with frequent complaints and adjust staffing or appointment templates accordingly.
- Leverage the AI appointment setter — Automatically schedule follow-ups for patients reporting poor experiences to prevent disengagement.
- Connect to the AI medical receptionist — Address recurring communication gaps between visits through automated outreach without adding staff workload.
Integrating patient flow solutions, such as automated scheduling and real-time tracking, can help streamline patient movement and reduce bottlenecks, making it easier to gather and act on feedback in a timely manner.
Step 6: Analyze Feedback Effectively
Collecting patient feedback without analyzing it systematically is like installing security cameras and never reviewing the footage. The data exists but produces no value without a process to turn responses into actionable insights.
Effective feedback analysis is not about reading every comment. It focuses on identifying patterns, measuring their frequency and impact, prioritizing them by operational significance, and presenting findings in a way that drives decisions.
How to analyze patient feedback effectively:
- Categorize feedback — Assign every score and comment to operational themes like wait times, provider communication, scheduling, staff attitude, billing, or facility to turn opinions into measurable intelligence.
- Track trends — Look at metrics over time, not just snapshots, to identify declining performance that requires immediate attention.
- Segment data — Break down results by provider, location, and visit type to uncover specific gaps hidden in practice-wide averages.
- Use sentiment analysis — Automate classification of open-ended comments as positive, negative, or neutral to identify recurring themes without manually reading every response.
- Correlate with operational data — Link feedback with scheduling, no-show rates, cancellations, and retention to understand how patient satisfaction affects operations.
- Set review cadence — Establish daily, weekly, monthly, and quarterly reviews with defined actions, from same-day follow-ups to strategic operational decisions.
Step 7: Act on Feedback & Close the Loop
This step separates clinics with a functional patient feedback system from those that just collect surveys. Collecting feedback without visible operational change signals to patients that their input is ignored, which can harm trust more than not collecting feedback at all.
Closing the loop means making operational changes based on feedback and communicating those changes to patients and staff so everyone sees real results.
How to act on feedback and close the loop effectively:
- Prioritize issues — Focus on problems that are frequent, impact retention or clinical outcomes, and can be addressed within current resources. Minor isolated complaints are lower priority.
- Contact dissatisfied patients quickly — Reach out within 24 hours to acknowledge their experience, apologize, and explain what the practice will do differently.
- Follow a structured service recovery script — Acknowledge the issue, apologize, explain actions taken to prevent recurrence, and offer a concrete next step like follow-up calls or priority scheduling.
- Assign owners and deadlines — Every improvement should have a specific person responsible and a completion date to ensure action.
- Communicate changes to patients — Inform patients who reported the issue about the improvement to show that feedback leads to real change.
- Announce improvements publicly — Share significant changes, such as extended hours or reduced wait times, via newsletters, website, or online profiles to enhance retention and acquisition.
- Track results — Monitor the feedback metric that prompted the change for four to eight weeks to confirm the improvement worked and adjust if needed.
- Share outcomes with staff — Present monthly summaries showing feedback received, improvements made, and measurable results to motivate staff and maintain the feedback system.
Example: “Thank you for your feedback! We have improved our scheduling process to reduce wait times and enhance communication with staff.”
How to Train Your Staff for Feedback Collection

A patient feedback system is only as effective as the people running it. The most sophisticated feedback technology produces poor results if staff do not know how to prompt patients naturally, recognize dissatisfaction signals, or escalate concerns to the right person at the right time.
Who needs to be trained:
- Front-desk staff — prompt patients to complete surveys at check-out, receive in-person complaints, and escalate unresolved concerns to the practice manager immediately
- Medical assistants and nurses — identify and flag dissatisfaction signals during rooming and pre-visit interactions; document verbal complaints for care coordinator follow-up
- Clinical providers — review individual satisfaction scores monthly; apply plain language communication and teach-back techniques that directly improve provider communication ratings
- Care coordinators — own the negative feedback escalation process; contact dissatisfied patients within 24 hours of a low-score submission
- Billing staff — handle billing-related complaints with transparency and empathy; escalate unresolved disputes before they generate negative online reviews
- Practice managers — review the daily feedback dashboard; present weekly trends at team huddles; hold staff accountable to response timeframes
How to train staff to prompt patients effectively:
- Teach a consistent check-out script such as “You will receive a short survey by text in the next couple of hours — it only takes a minute and your feedback genuinely helps us improve” — specific, warm, and purposeful.
- Train staff to make brief eye contact and pause after delivering the prompt rather than looking at a screen while the patient is gathering their belongings.
- Explain to staff why the feedback matters so they can communicate it authentically — patients who understand their input is reviewed and acted on are significantly more likely to complete surveys.
- Include feedback prompting in new hire orientation role-play exercises and quarterly refresher training so the prompt feels natural rather than scripted.
How to train staff to recognize and respond to in-person dissatisfaction:
- Train every patient-facing staff member to recognize verbal dissatisfaction signals including comments like “I have been waiting a long time,” “I am not sure I understood what the doctor said,” and “this is different from what I was told on the phone” — each is a feedback signal requiring an immediate empathetic response
- Teach the acknowledge-apologize-act framework: acknowledge the patient’s experience without minimizing it, apologize genuinely without making excuses, then act by resolving the issue on the spot or escalating it immediately
- Train staff to document every verbal complaint in the patient record with the date, nature of the concern, and action taken so patterns can be tracked and recurring issues identified
How to train staff on escalation protocols:
- Define a clear three-tier escalation structure — Tier 1 concerns such as wait time complaints and rescheduling requests are resolved by front-desk staff before the patient leaves; Tier 2 concerns such as staff behavior complaints and billing disputes require manager contact within two hours; Tier 3 concerns involving patient safety or provider misconduct require leadership notification within 30 minutes
- Train staff on exactly what information to capture before escalating — patient name, contact details, specific complaint, action already taken, and patient’s emotional state — so the receiving manager can respond effectively from the first contact
- Conduct monthly escalation audits reviewing whether issues were escalated at the correct tier, whether response timing met standards, and whether resolutions satisfied the patient
Recommended training cadence:
| Training Type | Frequency | Audience |
|---|---|---|
| New hire feedback orientation | At onboarding | All patient-facing roles |
| Check-out prompt refresher | Quarterly | Front-desk staff |
| Escalation protocol review | Quarterly | All staff |
| Provider feedback score review | Monthly | Clinical providers |
| Service recovery training | Bi-annually | Care coordinators and managers |
| Full system refresher | Annually | All staff |
Reporting Feedback Results to Leadership
Structured reporting helps leadership make data-driven decisions:
- Use dashboards and scorecards to track trends and recurring issues.
- Highlight improvements over time and measure outcomes of actions taken.
- Use reports to prioritize resource allocation, staff training, and process improvements.
Regular reporting fosters accountability and ensures clinics continually enhance care delivery quality.
Conclusion
A patient feedback system is essential for modern clinics. It provides a structured approach to capturing, analyzing, and acting on patient insights, leading to higher satisfaction, stronger patient-provider relationships, and improved operational efficiency.
When implemented correctly, it transforms patient input into actionable improvements, enhancing both care delivery and patient experience.
Clinics that listen and act on feedback build trust, encourage loyalty, and create a foundation for long-term growth. Starting small and integrating patient feedback into daily operations ensures ongoing improvements and measurable outcomes.
By embracing a structured feedback system, clinics can turn patient opinions into a strategic advantage, driving patient care improvement and operational excellence.
FAQs
What is a patient feedback system?
A patient feedback system is a structured process that collects, analyzes, and acts on patient input to improve care, operations, and overall patient experience.
Why should clinics collect patient feedback?
Clinics should collect patient feedback to identify areas for improvement, enhance patient experience, increase retention, and make data-driven operational and clinical decisions.
How often should patient feedback be collected?
Patient feedback should be collected at multiple intervals: after each visit for quick surveys, monthly or quarterly to track trends, and annually for an overall satisfaction review.
How do you increase survey response rates?
Keep surveys short, send promptly, personalize messages, use multiple channels, and explain the value.
What are the best ways to act on patient feedback?
Analyze trends, share insights with staff, implement changes, inform patients, and monitor improvements.
What is a healthcare feedback loop?
A healthcare feedback loop is a system that continuously collects patient feedback, analyzes it, and uses the insights to make operational or clinical improvements while communicating changes back to patients and staff.
How do you respond to negative patient feedback?
To respond to negative patient feedback, acknowledge the issue promptly, apologize sincerely, explain the corrective actions being taken, and follow up to ensure the patient’s concerns are addressed.



