Stop Charting After Hours. Start Documenting Smarter.
Your Clinic Is Losing Hours Every Day to Documentation That Shouldn't Take This Long
Clinicians didn’t train for years to spend their evenings catching up on charts.
But for most practices, that’s exactly what’s happening and the notes aren’t even better for it.
After-Hours Charting
Providers are finishing notes at 9pm that should have been done at 5pm. Every hour spent typing after clinic is an hour taken from rest, family, and the next day’s focus.
Incomplete or Vague Notes
Rushed documentation leads to missing details; functional limitations not recorded, prior treatments undocumented, care rationale unclear.
Coding Errors and Missed Revenue
When notes don’t clearly support the level of care delivered, coding teams either under-code to stay safe or spend hours chasing clinicians for clarification.
How Documentation Intelligence Works Across Your Entire Clinical Day
Because documentation shouldn’t slow down the work of care
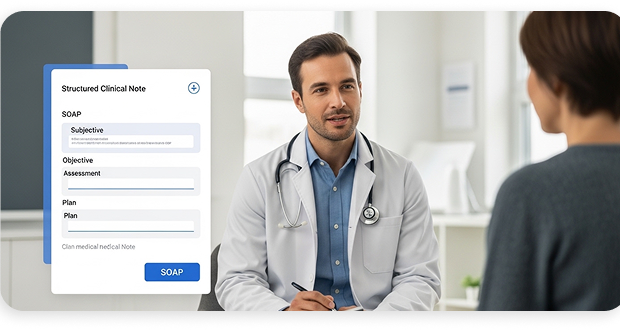
AI-Powered Clinical Note Generation
From Conversation to Structured Note
During every patient visit, our AI listens, understands context, and drafts a structured clinical note in real time. Subjective, objective, assessment, plan; all captured accurately so your provider can review, approve, and move on.
Medical Necessity & Prior Auth Support
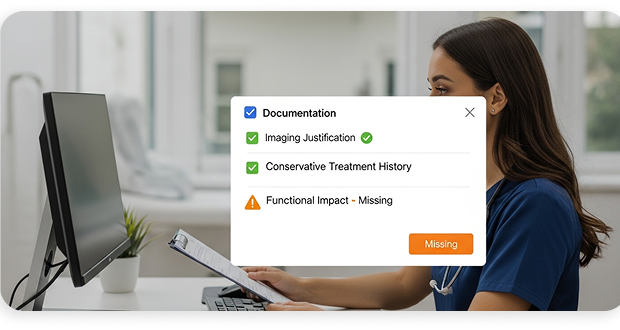
Surface What Insurers Need Before You Submit
Documentation Intelligence flags gaps in your notes before they become denials. If imaging justification is missing, if conservative treatment history isn’t documented, or if functional impact isn’t clearly stated; the system surfaces it at the point of care, not after a claim comes back rejected.
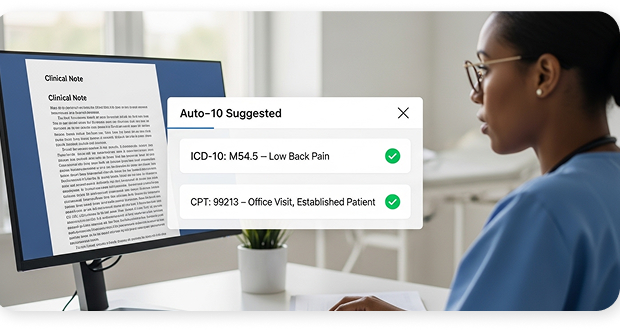
Structured Notes That Improve Coding Accuracy
Better Documentation Means Better Reimbursement
Every note generated is structured to support accurate ICD-10 and CPT coding. Coding teams get notes that are clear, complete, and consistent; reducing query time, reducing under-coding, and recovering revenue that was already earned but never captured.
This Is Built for You If Your Clinic Looks Like This
Three types of clinics. One shared problem
General Practice Clinics
Your GP shouldn’t be finishing charts at 9pm. Documentation Intelligence captures notes during the visit so the day ends when clinic does.
Specialty Clinics
Detailed requirements, prior auth pressure, and documentation that has to hold up clinically and financially. Documentation Intelligence makes sure.
Allied Health Clinics
When notes drive outcomes and reimbursement equally, consistency matters. Our AI keeps documentation complete across your entire team.
What Documentation Intelligence Does for Your Practice
Every clinic at your stage has the same breaking points. Here’s where the time and revenue are quietly disappearing.
More Time with Patients
Providers stop typing during visits and start being fully present; better care, better experience, better outcomes.
Evenings Back
No more after-hours charting. Notes are ready to review and approve before the last patient leaves.
Fewer Prior Auth Denials
Real-time gap flagging means the right details are in the note before submission, not discovered after a rejection.
Recovered Coding Revenue
Consistently structured notes reduce under-coding and billing queries, capturing reimbursement you’ve already earned.
HIPAA-Compliant by Design
Every interaction is encrypted, role-access controlled, and built to meet the highest standards of patient data protection.
Plugs Into Your EHR
Documentation Intelligence integrates directly into your current practice setup with no steep learning curve.
Why Medlaunch for Healthcare IT Solutions?
Deep Healthcare Industry Expertise
Use automated workflows to streamline intake, routing, and provider assignments.
End-to-End Digital Solution Implementation
We manage your complete healthcare solution setup and long-term support.
AI-Enabled Automation Tools
We deliver AI automation that reduces admin work, delays, and no-shows while giving providers actionable insights.
Connected Healthcare Ecosystem
With 10+ years of experience, we deliver HIPAA-aligned solutions built for real GP and specialty clinic workflows.
Customizable and Scalable Clinic Solutions
Every solution scales with your clinic’s evolving needs, supporting staff and new services as you expand.
Frequently Asked Questions
Still Have Questions? Good. Here Are the Honest Answers.
Yes, with explicit consent protocols built into the workflow. The system captures the clinical conversation during the visit using ambient audio technology to generate a structured note in real time. Patient privacy and HIPAA compliance are enforced at every step through encrypted data transmission and role-based access controls. Importantly, audio recordings are not retained after the note has been generated. Only the structured clinical note remains.
Yes. Before go-live, MedLaunch configures AI Clinical Documentation for Healthcare Clinics to your specific note templates, preferred clinical language, and documentation structure. The system generates notes that read and feel consistent with how your providers already document, not like generic AI output. Configuration is handled entirely by our team before your first live session.
The system is trained to identify documentation gaps that commonly trigger prior authorisation delays or denials. These include missing functional impact statements, undocumented conservative treatment history, unclear medical necessity rationale, and absent chronological pain progression. When a gap is detected, the system surfaces it at the point of note approval, before you sign, not after a claim comes back rejected.
Most clinics are fully live within two to four weeks. MedLaunch handles the entire setup process: EHR integration, note template configuration, clinical language customisation, and staff briefing. The clinic's involvement during setup is minimal. Your team does not need to manage any technical configuration.
AI Clinical Documentation for Healthcare Clinics generates SOAP notes (Subjective, Objective, Assessment, Plan) and can be configured for other structured note formats used in GP, specialty, and allied health settings. Every note includes the relevant clinical sections your EHR and billing team requires, structured for accurate ICD-10 and CPT coding support.
AI Clinical Documentation for Healthcare Clinics is configured to integrate with your clinic's existing EHR system as part of the setup process. MedLaunch manages the integration on your behalf. If you are evaluating whether your specific EHR is supported, contact us before committing and we will confirm compatibility and integration scope upfront. Currently integratable with Epic and Athena Health.
All patient data processed by AI Clinical Documentation for Healthcare Clinics is encrypted in transit and at rest. The system operates within a HIPAA-aligned framework that includes role-based access controls, audit logging, and a Business Associate Agreement with MedLaunch. Audio is not retained after the clinical note is generated. No patient data is used to train external models.
Yes. AI Clinical Documentation for Healthcare Clinics supports multi-provider environments. Each provider has their own access credentials and note approval workflow. Notes are generated, reviewed, and approved per provider, and the system can be configured with provider-specific language preferences and note templates within the same clinic setup.
Every note is presented to the provider for review and approval before it is finalised. No note is automatically added to the patient record. The provider reads, edits if needed, and approves. The system is a documentation assistant, not an autonomous documenter. Clinical judgment and the provider's sign-off remain the final step in every case.
