PHQ-9 longitudinal tracking is the systematic re-administration of the Patient Health Questionnaire-9 at defined intervals throughout a patient’s treatment episode, with each score recorded, trended over time, and used to guide clinical decision-making at every visit. It is not the same as one-time depression screening. A single PHQ-9 score tells a clinician whether depression is present and how severe it appears at that moment. A longitudinal track of PHQ-9 scores across multiple visits tells a clinician whether the treatment is working, whether it has stopped working, whether the patient is approaching remission, and whether the clinical decision made at the last visit produced the outcome it was intended to produce.
This blog explains what PHQ-9 longitudinal tracking is, why the clinical evidence for measurement-based care is stronger than most clinicians realise, what happens to treatment outcomes when tracking is absent, how AI-powered PHQ-9 screening makes longitudinal tracking operationally viable in a small clinic, and what the five clinical decisions that longitudinal tracking enables look like in practice.
Key Takeaways: The Clinical and Operational Power of PHQ-9 Tracking
-
1Remission Rates and MBC: Measurement-based care (MBC) using structured PHQ-9 tracking produces remission rates of 52.8%, compared to just 43.0% in standard care. The difference is not the treatment itself, but the session-by-session objective data guiding clinical adjustments.
-
2The MBC Performance Gap: Landmark RCT data shows that patients receiving structured MBC achieve a 74% remission rate over 24 weeks, whereas standard care results in only 29%. This nearly triple improvement highlights the failure of relying solely on ad hoc clinical assessments.
-
3Faster Recovery Timelines: A 2025 JAMA Network Open study found that time to remission was cut in half when MBC replaced standard care. Faster response means fewer weeks of active symptoms and fewer visits required before documenting meaningful improvement.
-
4Guideline Non-Adherence: Despite proven benefits, only 28.2% of depression treatment episodes include a PHQ-9 within the first 60 days. Most clinical episodes proceed without structured tracking, representing a massive gap between evidence-based guidelines and actual practice.
-
5The Failure of Paper Tracking: Paper forms cannot sustain longitudinal tracking at scale. Effective MBC requires automated delivery, structured score storage, trend visualization, and plateau alerts—operational capabilities that manual systems simply cannot provide for a busy panel.
Table of Contents
What Is PHQ-9 Longitudinal Tracking and How Is It Different from One-Time Screening?
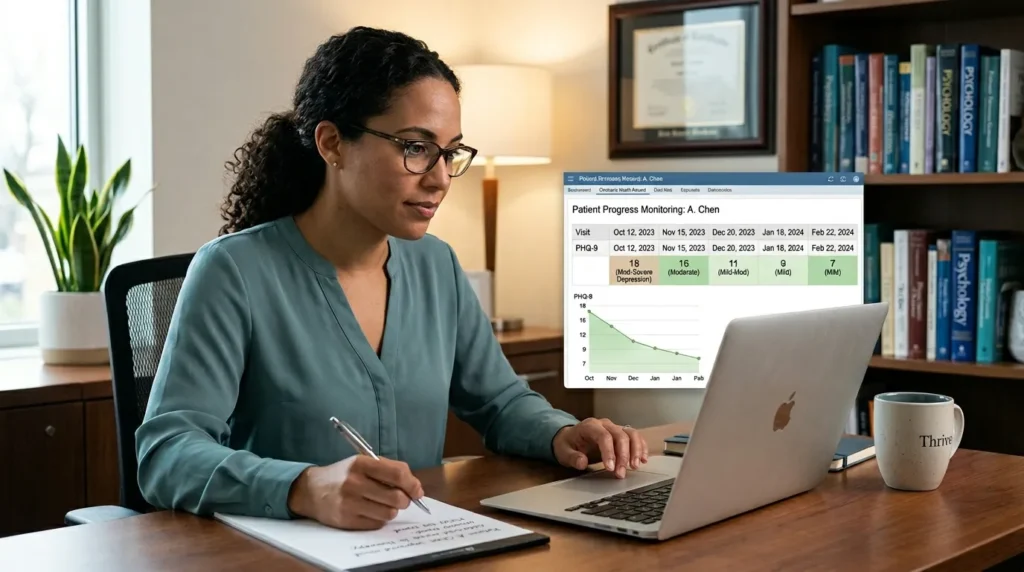
PHQ-9 screening and PHQ-9 longitudinal tracking are related but clinically distinct functions. Understanding the difference is essential for understanding why longitudinal tracking changes treatment outcomes in ways that one-time screening cannot.
One-time PHQ-9 screening answers one question: does this patient currently have depressive symptoms, and if so, how severe are they? A score of 10 or above has 88% sensitivity and 88% specificity for major depressive disorder. The screening identifies the patient. It establishes a baseline. It triggers the initial clinical response, whether that is watchful waiting, initiating antidepressant therapy, referring to a therapist, or a combination. One-time screening is a diagnostic and triage function.
PHQ-9 longitudinal tracking answers a different and more clinically actionable set of questions: is this patient’s score improving, stable, or worsening since the last visit? Is the rate of improvement consistent with what the literature suggests for the treatment being used? Has the score crossed the 50% reduction threshold that defines treatment response? Has the score fallen below 5, which defines remission? Is the patient who appeared to be improving last month now scoring higher than they were two months ago?
These questions cannot be answered from a single score. They require a time series. The PHQ-9’s minimal clinically important difference for individual change is 5 points on the 0 to 27 point scale, according to research from the IMPACT study. A score change of less than 5 points between visits may represent measurement variability rather than genuine clinical change. A score change of 5 points or more in either direction represents a clinically meaningful signal that warrants a treatment decision.
Without longitudinal tracking, that signal is invisible.
Why Do Clinicians Underestimate Treatment Inadequacy Without PHQ-9 Data?
One of the most consistent findings in the clinical literature on depression management is that clinicians systematically overestimate how well their patients are responding to treatment when they rely on clinical global impression rather than structured outcome measurement.
A study examining concordance between PHQ-9 scores and physician assessment at urban primary care settings found that Cohen’s Kappa analysis showed only slight agreement between depression symptoms documented by PHQ-9 and physician-documented symptoms during the same clinical encounter, with agreement values between 0.001 and 0.101 across all depression symptom domains. The agreement between what the PHQ-9 measured and what the physician documented was, in statistical terms, barely above chance.
A qualitative study published in a British Journal of General Practice cohort, examining discrepancies between PHQ-9 scores and patients’ global rating of change, found that 51% of cases showed a mismatch between PHQ-9 score trajectory and both patient and clinician global impression of change. In half of all cases, the objective score and the subjective clinical impression were pointing in different directions.
This is not a failure of clinical competence. It is a structural feature of depression assessment without structured measurement. Depression presents through subjective patient reporting in a brief appointment. The patient who has learned to present positively, the patient whose somatic symptoms persist even as mood improves, the patient whose functional impairment remains high while their PHQ-9 score has technically crossed the response threshold, all of these presentations create discordance between the objective score and the clinical impression that cannot be resolved without the score.
PHQ-9 longitudinal tracking gives the clinician an objective anchor for every treatment decision. Not a replacement for clinical judgement. An input to it that is otherwise unavailable.
The Five Clinical Decisions That PHQ-9 Longitudinal Tracking Enables

The clinical value of longitudinal PHQ-9 tracking is most clearly understood through the specific decisions it enables at each phase of treatment. These are decisions that clinical global assessment alone cannot reliably support.
Decision 1: Whether to initiate or defer treatment at the first clinical contact. A first PHQ-9 score establishes the severity baseline. A score between 10 and 14 (moderate) and a score between 15 and 19 (moderately severe) warrant different initial responses. A score of 10 at first contact that is tracked two weeks later and scores 14 is clinically different from a score that has fallen to 7 in the same period. Without a second measurement, the clinician cannot distinguish between a worsening trajectory and an improving one at what appears to be the same severity level on first presentation.
Decision 2: Whether to continue, adjust, or change a treatment at the 4 to 8 week review. Antidepressant response typically begins to appear at 4 to 6 weeks. If a patient started on antidepressant therapy with a PHQ-9 of 16 and attends the 6-week review still scoring 14, a 2-point reduction below the 5-point minimum clinically important difference may not represent genuine treatment response. Without the longitudinal score, the clinician has only the patient’s subjective report and their own clinical impression. With the longitudinal score, the clinician has an objective measure of whether the treatment threshold for response has been crossed.
Decision 3: Whether a patient who appears stable has actually reached remission. Remission in depression is defined as a PHQ-9 score below 5 sustained across multiple visits. A patient who is “doing much better” by clinical global impression may be scoring 8 or 9, which represents residual symptoms significantly associated with higher relapse risk than a score below 5. The difference between a patient at remission and a patient with residual symptoms is not reliably detectable from clinical impression alone. It is detectable from the score.
Decision 4: Whether a patient who is improving is improving fast enough. The 2025 JAMA Network Open RCT found that MBC cuts time to response and remission in half compared to standard care. The mechanism is not that MBC makes the medication work faster. It is that structured PHQ-9 tracking gives clinicians the objective data to identify when a treatment is not producing adequate response at the expected rate and to make earlier adjustments. Clinicians without longitudinal PHQ-9 data wait longer before recognising inadequate response because they rely on clinical impression, which systematically underestimates treatment inadequacy.
Decision 5: Whether a patient who has achieved remission is at risk of relapse. Longitudinal tracking does not stop at remission. It continues through the maintenance phase of treatment and detects early score increases that precede clinical relapse. A patient who achieved remission with a PHQ-9 of 3 and is now scoring 7 at a routine follow-up may not be presenting with overt depressive symptoms. The score increase is a leading indicator of relapse that appears before the clinical presentation does. Without the longitudinal track, that indicator is invisible until the relapse is fully established.
What Longitudinal PHQ-9 Tracking Looks Like in Practice: Three Patient Scenarios
The following three scenarios show the same clinical situation at two different points in a treatment episode, with and without longitudinal PHQ-9 data available to the clinician.
Scenario 1: The patient who appears to be responding but is not
Without longitudinal tracking: Patient attends 8-week review. Reports feeling “somewhat better.” Clinician notes improved affect and continued compliance. Treatment continued unchanged.
With longitudinal tracking: PHQ-9 at intake was 17. PHQ-9 at 4 weeks was 15. PHQ-9 at 8 weeks is 14. Total reduction of 3 points over 8 weeks, below the 5-point minimal clinically important difference. The score trend shows a plateau rather than a response trajectory. Clinician has objective evidence to consider dose adjustment or treatment augmentation at 8 weeks rather than waiting until week 16 or 24.
Scenario 2: The patient who appears stable but has reached remission
Without longitudinal tracking: Patient attends 6-month review. Appears well. Reports feeling “back to normal.” Clinician schedules next review in 3 months. Treatment continuation discussed informally.
With longitudinal tracking: PHQ-9 at intake was 16. PHQ-9 across 6 months shows a trajectory of 16, 13, 9, 6, 4, 3. Remission defined as below 5 was achieved at month 4 and has been sustained for 2 months. Clinician has objective evidence to initiate a structured maintenance phase conversation, discuss antidepressant taper options, and document remission in the clinical record with the score data that supports the clinical decision.
Scenario 3: The patient who is relapsing between visits
Without longitudinal tracking: Patient who achieved remission 6 months ago attends for an unrelated complaint. Does not mention mood. Clinician does not ask. Relapse not detected.
With longitudinal tracking: Automated PHQ-9 delivered pre-visit as part of standard intake protocol. Score at today’s visit is 9, up from 3 at last depression-related visit 3 months ago. Alert surfaced in EHR before the appointment. Clinician addresses mood in the consultation. Early relapse detected and managed before it becomes a full depressive episode.
For clinics combining PHQ-9 longitudinal tracking with AI clinical documentation, the AI clinical documentation implementation timeline explains how both tools integrate within the same EHR environment.
Why a Paper PHQ-9 Cannot Support Longitudinal Tracking at a Clinic Level

The clinical case for PHQ-9 longitudinal tracking is strong. The operational reason it is not widely implemented in small clinics is equally clear: a paper PHQ-9 cannot do it.
Sustaining longitudinal PHQ-9 tracking across a panel of patients with depression in a small clinic requires four operational capabilities that paper forms do not provide.
Automated session-by-session delivery. A paper form requires a staff member to remember to give it to the right patient at the right visit, at the correct interval based on that patient’s treatment phase. Across a panel of 20 or 30 patients with depression at various stages of treatment, each requiring a different reassessment interval, this is not a reliable manual process. It is a system requirement.
Structured score storage with trend calculation. A paper PHQ-9 score entered manually into a free-text EHR note cannot be trended. It cannot trigger a comparison to the previous score. It cannot calculate whether the change exceeds the 5-point minimal clinically important difference. It is a number in a document, not a data point in a longitudinal series.
Clinician alert on score change or plateau. The clinical value of longitudinal tracking is not the score itself. It is the change in the score and the alert when that change signals a clinical decision point. A system that stores scores but does not surface an alert when a score has not moved by 5 points in 8 weeks does not deliver the clinical benefit of MBC. Paper cannot surface that alert. An automated system can.
Population-level visibility across all patients with depression. In a small clinic, the clinician who can see at a glance which patients in their depression panel have not had a PHQ-9 in 60 days, which are approaching the response threshold, and which have scores trending upward toward relapse is in a fundamentally different clinical position from the clinician who has to check each patient’s paper record individually to reconstruct that picture.
A 2025 retrospective cohort study from Karolinska Institutet found that only 28.2% of depression treatment episodes included any PHQ-9 or outcome measure within 60 days of treatment initiation. The paper-based and ad hoc delivery systems currently in place are not producing guideline-concordant outcome measurement. They are producing 28.2% adherence.
AI-powered PHQ-9 systems deliver all four operational capabilities. The PHQ-9 is sent automatically at the correct interval for each patient based on their treatment phase. Scores are stored in a structured database and trended automatically. Clinician alerts surface when scores change, plateau, or worsen beyond the clinically meaningful threshold. Population-level dashboards show every patient with depression in the panel, their current score, their trend, and when their next assessment is due.
Without PHQ-9 Longitudinal Tracking vs With PHQ-9 Longitudinal Tracking
Without longitudinal tracking:
- Treatment initiated based on first PHQ-9 score and clinical impression
- 4 to 8 week review conducted based on patient-reported subjective improvement
- Clinician relies on global clinical impression for treatment continuation decisions
- Inadequate treatment response detected late, often at 12 to 24 weeks
- Remission status undocumented or based on patient self-report
- Early relapse signals missed between scheduled appointments
- 28.2% of treatment episodes include any structured outcome measurement
- Remission rates of approximately 29% to 43% in standard care conditions
With AI-powered PHQ-9 longitudinal tracking:
- Treatment initiated with baseline score established and stored automatically
- PHQ-9 delivered automatically at correct interval, pre-visit, completed before appointment
- Score trend available in EHR before every relevant appointment
- Clinician alerted when score change is below minimal clinically important difference at 8 weeks
- Remission documented with objective score data at the point it is achieved
- Early relapse detected from score trend before clinical presentation deteriorates
- 100% of depression panel patients tracked systematically without staff administration burden
- Remission rates of 52.8% to 74% in MBC conditions across multiple RCTs
The compounding outcome: A small clinic with 30 patients with depression in treatment, converting from ad hoc paper-based PHQ-9 to AI-powered longitudinal tracking, can expect to identify inadequate treatment response earlier, adjust treatment sooner, achieve remission at a meaningfully higher rate, and detect early relapse before it becomes a full depressive episode, based on the consistent finding across multiple RCTs that MBC produces remission rates approximately 10 to 45 percentage points higher than standard care.
What This Means for Clinics Implementing PHQ-9 Longitudinal Tracking in 2026
The evidence for MBC is now at the level of multiple RCTs, not observational studies. The 2025 JAMA Network Open RCT, the systematic review and meta-analysis in the Journal of Clinical Psychiatry, and the landmark 24-week RCT showing 74% versus 29% remission rates are not pilot studies or single-site observations. They are controlled trials at a level of evidence that changes the clinical standard. Treating depression without structured PHQ-9 longitudinal tracking in 2026 is treating depression without the intervention that the evidence most consistently associates with better outcomes.
The operational gap is now closable for small clinics. Until AI-powered PHQ-9 systems existed, sustained longitudinal tracking in a small clinic was a systems problem that most practices could not solve with paper forms and manual reminders. That gap has closed. Automated pre-visit delivery, structured score storage, trend alerts, and population dashboards are available in systems that integrate natively with Epic and Athena Health and configure to a small clinic workflow in days rather than months.
The minimal clinically important difference of 5 points is the key number for every review. At every treatment review, the question the longitudinal PHQ-9 score should answer is: has this score changed by 5 or more points since the last assessment? If yes, in which direction? If no, for how many consecutive assessments? That 5-point threshold is the objective anchor for every treatment continuation, adjustment, and escalation decision. It does not replace clinical judgement. It informs it with data that clinical impression alone cannot provide.
Documentation of longitudinal PHQ-9 scores supports billing and quality reporting. For clinics participating in MIPS quality reporting, documented PHQ-9 longitudinal tracking with follow-up scores generates structured quality measure data across the depression panel. For clinics operating under value-based care contracts, documented remission rates and treatment response rates derived from longitudinal PHQ-9 data are the evidence that care quality can be measured against.
For GP clinics implementing PHQ-9 screening for the first time, the operational foundation for longitudinal tracking starts with systematic primary care PHQ-9 screening, covered in detail in AI PHQ-9 screening for primary care.
MedLaunch AI Powered PHQ-9 Screening delivers longitudinal PHQ-9 tracking as a built-in clinical workflow. Automated pre-visit delivery at configured intervals. Session-by-session score storage and trend calculation. Clinician alerts when scores plateau, worsen, or reach response and remission thresholds. Population-level depression panel visibility within Epic and Athena Health. Configuration to clinic-specific reassessment intervals before go-live.
The full workflow is on the AI Powered PHQ-9 Screening solution page.
Frequently Asked Questions
What is PHQ-9 longitudinal tracking?
PHQ-9 longitudinal tracking is the systematic re-administration of the Patient Health Questionnaire-9 at defined intervals throughout a patient’s treatment episode, with each score recorded, trended over time, and used to guide clinical decision-making at every visit. It is the core operational mechanism of measurement-based care for depression. A single PHQ-9 identifies whether depression is present. A longitudinal PHQ-9 track tells the clinician whether the treatment is producing the expected response, whether the patient is approaching remission, and whether clinical decisions made at previous visits were effective.
What does the evidence say about PHQ-9 longitudinal tracking and treatment outcomes?
The evidence is consistent across multiple randomised controlled trials. A systematic review and meta-analysis published in the Journal of Clinical Psychiatry found remission rates of 52.8% for MBC versus 43.0% for standard care across five RCTs with 1,518 participants. A landmark 24-week RCT found 74% remission in the MBC group versus 29% in standard care. A 2025 JAMA Network Open RCT found that time to response and time to remission were cut in half with MBC compared to standard care. The consistent finding across these trials is that structured outcome measurement using PHQ-9 tracking, rather than clinical global assessment alone, is associated with significantly better treatment outcomes.
What is the minimal clinically important difference for the PHQ-9?
The minimal clinically important difference for the PHQ-9 is 5 points on the 0 to 27 point scale, based on research from the IMPACT study examining responsiveness to treatment in late-life depression. A score change of less than 5 points between visits may represent measurement variability rather than genuine clinical change. A score change of 5 points or more represents a clinically meaningful signal that warrants a treatment decision, whether that is continuing the current approach because it is working or adjusting the treatment because it is not.
How does PHQ-9 longitudinal tracking differ from one-time depression screening?
One-time PHQ-9 screening identifies whether a patient currently has depressive symptoms and how severe they are. It is a diagnostic and triage function. PHQ-9 longitudinal tracking monitors whether a treatment is working, whether the patient is approaching or has reached remission, whether a treatment that appeared to be working has plateaued below the response threshold, and whether a patient in remission is showing early signs of relapse. These are treatment management functions that require a time series of scores, not a single measurement.
Why do most clinics not implement PHQ-9 longitudinal tracking systematically?
The primary barrier is operational. Sustaining longitudinal PHQ-9 tracking across a panel of patients at various treatment stages requires automated session-by-session delivery, structured score storage with trend calculation, clinician alerts on score change or plateau, and population-level visibility. Paper forms and manual reminder systems cannot deliver these capabilities reliably at a small clinic level. A 2025 retrospective cohort study from Karolinska Institutet found that only 28.2% of depression treatment episodes included any structured outcome measurement within 60 days of treatment initiation, despite clinical guidelines recommending it. The gap is not clinical disagreement. It is operational infrastructure.
What is treatment response and remission in PHQ-9 terms?
Treatment response is defined as a 50% or greater reduction in PHQ-9 score from baseline, according to research published in Psychiatric Services examining outcome definitions across 5,554 psychotherapy episodes. A patient who started at a PHQ-9 of 16 and is now scoring 8 or below has reached the response threshold. Remission is defined as a PHQ-9 score below 5, sustained across multiple visits. The distinction between response and remission matters clinically because patients who have responded but not remitted, scoring between 5 and 9, have significantly higher relapse risk than patients who have achieved full remission. Longitudinal tracking makes both thresholds visible and documentable.
Can AI-powered PHQ-9 systems deliver longitudinal tracking for a small clinic? Yes. AI-powered PHQ-9 systems deliver automated pre-visit delivery at configured intervals, structured score storage and trend calculation, clinician alerts when scores plateau, worsen, or cross response and remission thresholds, and population-level depression panel visibility. These are the four operational capabilities that paper forms cannot provide and that small clinics without dedicated care coordination staff cannot sustain manually. The same system that delivers baseline screening at the first visit automatically schedules and delivers the follow-up assessments based on the configured reassessment interval for that patient’s treatment phase.
Conclusion
The gap between what PHQ-9 longitudinal tracking produces and what standard care without it produces is not a marginal clinical improvement. It is a 74% versus 29% remission rate in one landmark trial. It is time to response and remission cut in half in a 2025 RCT. It is a response rate advantage of 4.9 percentage points and a remission rate advantage of 9.8 percentage points in a systematic review of five trials with more than 1,500 patients.
The evidence has been building for over a decade and is now at the level of multiple randomised controlled trials with consistent findings across different clinical populations, different countries, and different treatment settings. Structured PHQ-9 tracking across visits is not a quality improvement aspiration. It is the specific intervention that the clinical literature associates most consistently with better depression treatment outcomes.
The reason it is not universally implemented is operational. A paper PHQ-9 cannot be automatically delivered at the correct interval. It cannot store a score trend. It cannot alert the clinician when a patient has not improved by the minimal clinically important difference in eight weeks. It cannot show a population-level view of which patients in the depression panel are approaching remission and which are not responding.
AI-powered PHQ-9 systems can do all of these things. The operational gap that has kept longitudinal tracking out of small clinic practice is now closable. The clinical case for closing it has never been stronger.
A single PHQ-9 detects depression. A track tells you if treatment is working.
MedLaunch delivers automated session-by-session tracking, score trend alerts, and panel visibility within your EHR. See the full longitudinal workflow on our solution page.



