Key Takeaways
-
1Revenue Growth: Revenue growth does not always require more patients. Fixing billing errors, reducing no-shows, and improving collections can recover lost income.
-
2No-Show Costs: No-shows cost the U.S. healthcare system about $150 billion annually. Automated reminders and easy rescheduling can significantly reduce missed visits.
-
3Denial Management: With denial rates around 10–15%, accurate coding, timely claims, and denial management are critical for healthy cash flow.
-
4Specialty Specifics: Each specialty has different revenue drivers, so focusing on practice-specific strategies improves financial results.
-
5Reminder Automation: Automation for reminders, insurance checks, and claims reduces errors, saves staff time, and captures more billable services.
Growing medical practice revenue is the key to keeping your clinic healthy and running smoothly. But many practices lose money every day, not because they don’t have enough patients, but because of missed chances, billing mistakes, and patients who don’t come back.
Running a clinic today is harder than ever. Costs keep going up, insurance payments are complicated, and patients expect more from their experience. All of this makes finding effective ways to increase medical practice revenue feel like an uphill battle.
The good news is that seeing more patients is not the only answer. With the right mix of better scheduling, smarter billing, stronger patient relationships, and simple automation, clinics can grow their revenue without working harder than they already do.
In this guide we break down what drives revenue in a medical practice, the most common challenges clinics face, and 10 simple ways to increase practice revenue for a medical practice without burning out your team.
Table of Contents
What Drives Revenue in a Medical Practice?
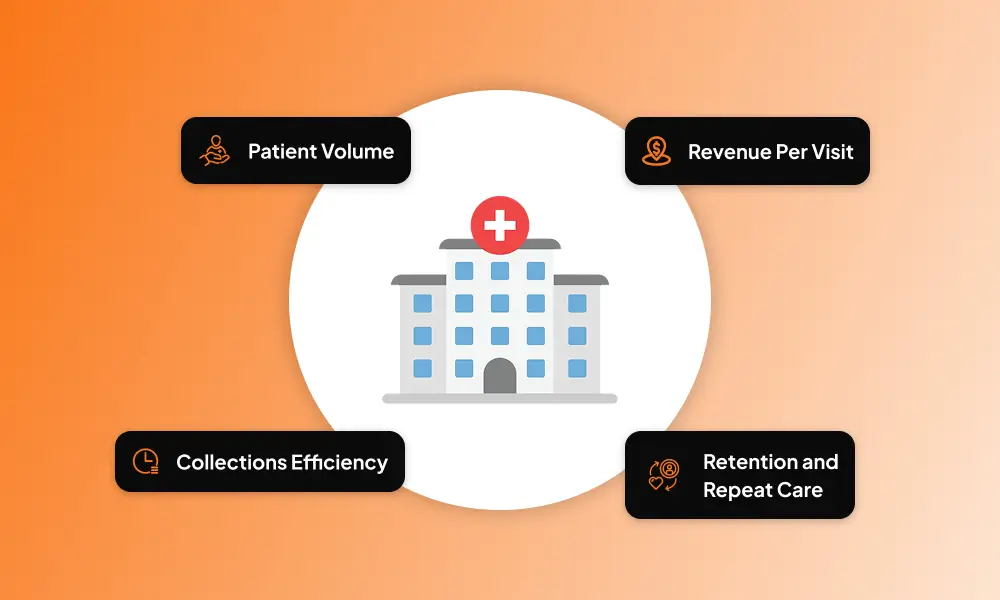
Revenue in a medical practice comes from multiple sources, and understanding these drivers is essential for long-term growth.
Core Revenue Levers
- Patient Volume: Bringing in new patients is important, but maintaining a steady flow of returning patients is even more critical. Repeat visits contribute to ongoing revenue and strengthen patient relationships.
- Revenue Per Visit: The amount collected per visit depends on services offered, insurance reimbursements, and patient co-pays. Offering preventive screenings or optional add-on services increases revenue without extending office hours.
- Collections Efficiency: Timely billing, accurate coding, and consistent follow-up ensure that the practice receives payment on time, minimizing revenue leakage.
- Retention and Repeat Care: Encouraging patients to return for follow-ups and preventive care increases their lifetime value and reduces marketing costs for acquiring new patients.
Why Revenue Growth Is Multi-Factor
Revenue growth is rarely achieved with a single strategy. Practices that optimize operations, reduce errors in billing, and focus on patient retention tend to see long-term success.
Around 19% of healthcare organizations report losing 20% of revenue due to poor patient retention, and 43% say poor retention costs them over 10% of revenue.
True practice profitability requires balancing operational efficiency, quality care, and smart revenue management. Clinics that track metrics like reimbursement rates, denials, and patient lifetime value are better positioned to grow sustainably.
Common Revenue Challenges Faced by Medical Practices

Even well-managed clinics face hurdles that impact financial performance:
- Claims Denials: Coding errors, incomplete documentation, or insurance verification issues can delay or prevent reimbursement. Denials that are not addressed promptly often become lost revenue.
- Appointment No-Shows: Empty slots reduce staff efficiency, frustrate patients, and decrease revenue.
- Revenue Leakage: Unbilled services, missed charges, and delayed collections often remain unnoticed until they significantly impact profits.
- Limited Insights: Without data, clinics cannot identify which services or patient segments are most profitable, limiting opportunities to optimize revenue.
Identifying these challenges is the first step toward addressing them effectively with patient flow solutions.
10 Proven Revenue-Growth Strategies
There are multiple strategies you can implement to achieve revenue growth, and using a combination of these can have a significant impact on your practice’s profitability.
Here are the 10 time-tested ways to increase medical practice revenue, streamline operations, and boost patient satisfaction.
Strategy 1: Reduce Missed Appointments and No-Shows
Missed appointments are one of the largest sources of lost revenue in medical practices.
Effective approaches include:
- Automated reminders via SMS, email, or phone, reducing no-show rates by up to 30%.
- Flexible scheduling, including same-day appointments and waitlists.
- Personalized follow-up calls for patients with chronic conditions or critical follow-ups.
- Charging small fees for missed appointments or offering incentives for timely visits can also improve attendance.
Patient no‑shows cost the U.S. healthcare system about $150 billion per year, and individual practices can lose around $150,000 annually from empty slots.
Strategy 2: Improve Patient Retention and Repeat Visits
Keeping patients engaged reduces marketing costs and increases revenue. Repeat visits also improve patient lifetime value.
Ways to encourage retention:
- Schedule follow-up appointments during the current visit.
- Send reminders for preventive care, annual check-ups, or lab work.
- Educate patients about their treatment plans.
- Offer wellness or loyalty programs to incentivize continuous care.
Example: A family practice implemented a preventive care program with automated reminders for vaccinations and screenings.
Across published studies, automated reminders reduce no‑shows by about 29%, while manual phone calls cut them by roughly 39% of the baseline no‑show rate, demonstrating strong effectiveness for both approaches.
Strategy 3: Optimize Revenue Cycle Management
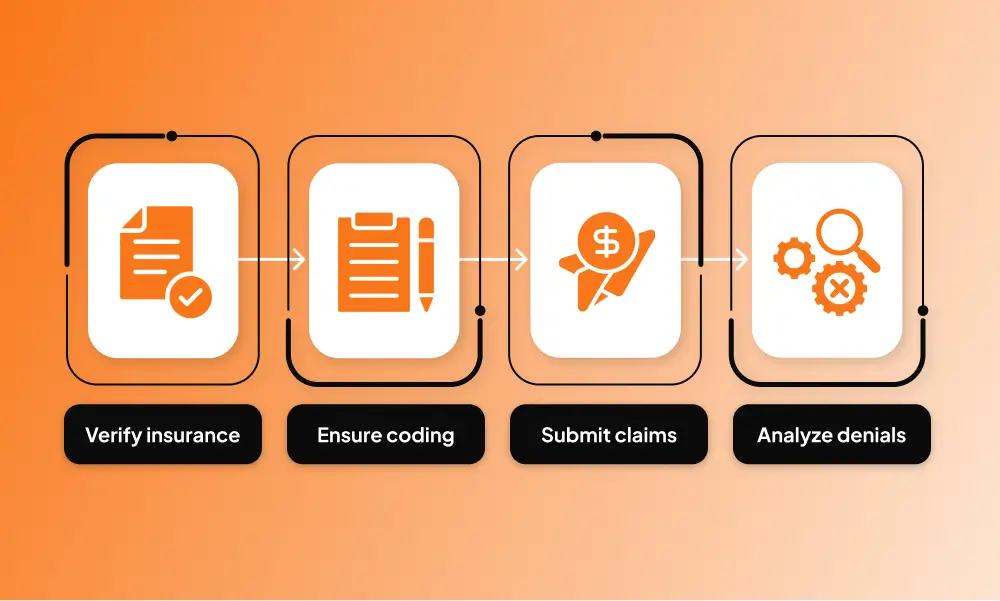
A smooth revenue cycle ensures that services are billed accurately and paid promptly.
Steps for optimization:
- Verify insurance coverage before the patient visit.
- Ensure coding is accurate and documentation is complete.
- Submit claims promptly and track unpaid balances.
- Analyze denials and implement corrective measures.
Rising denial rates now reach 10–15% for many providers, contributing to an estimated $262 billion in annual lost revenue and rework costs across U.S. healthcare.
Advanced software can automate some of these steps, helping clinics reduce claims denial rates and accelerate collections. Practices that invest in healthcare revenue optimization often recover thousands in lost revenue annually.
Strategy 4: Increase Revenue Per Patient Visit
Maximizing revenue per visit increases profitability without increasing patient volume.
Tactics include:
- Ensure all billable services are captured through medical billing optimization.
- Offer additional preventive services or chronic care management programs.
- Use bundled service packages to increase efficiency and reimbursement.
Even a small increase in revenue per patient can compound significantly over months. For example, offering a diabetes management package or annual wellness check-ups can generate additional revenue while improving patient health.
Strategy 5: Expand or Refine High-Margin Services

High-margin services, such as lab testing, specialty procedures, or imaging, generate substantial revenue relative to their cost.
Implementation tips:
- Identify services with strong reimbursement and low operational cost.
- Train staff to identify opportunities to offer these services.
- Educate patients on available high-value services.
Focusing on high-margin offerings diversifies revenue streams and supports financial stability, contributing to sustainable practice profitability.
Strategy 6: Improve Pricing and Payer Mix
Not all insurance payers reimburse at the same rate. Optimizing your payer mix ensures timely, fair payments and reduces revenue risk.
Best practices:
- Review contracts to prioritize high-performing payers.
- Focus on payers with low denial rates and timely reimbursement.
- Adjust service pricing where appropriate while staying competitive.
A well-managed payer strategy protects revenue and strengthens long-term clinic revenue strategies.
Strategy 7: Strengthen Front-Desk and Scheduling Performance
The front desk is critical to capturing revenue. Inefficiencies in registration, insurance verification, and scheduling can result in lost revenue.
Ways to improve:
- Train staff to accurately collect patient and insurance information.
- Monitor appointment efficiency and follow up on missed visits.
- Use scheduling software to optimize workflow and reduce wait times.
An efficient front desk, combined with AI patient scheduling, improves patient experience, reduces appointment no-shows, and minimizes revenue leakage.
Strategy 8: Recover Revenue Lost to Operational Gaps

Revenue may be lost due to unbilled services, missed follow-ups, or partial payments.
Strategies:
- Conduct audits to find missed or incorrectly billed services.
- Track all services to ensure accurate billing.
- Follow up on unpaid or partially paid claims.
Operational improvements can significantly increase cash flow without adding new patients.
Strategy 9: Use Data to Track and Improve Revenue Performance
Data-driven decisions improve clinic performance and revenue.
Metrics to monitor:
- Days in accounts receivable
- Denial rates and reasons
- Appointment attendance rates
- Revenue per service type
- Patient lifetime value
Tracking these metrics allows clinics to identify revenue opportunities, optimize workflows, and enhance healthcare profitability.
Strategy 10: Leverage Automation and Systems
Automation reduces errors, frees staff time, and ensures consistent billing.
Automation opportunities:
- Insurance verification
- Appointment reminders
- Claims submission and tracking
- Payment posting
Healthcare automation solutions allow staff to focus on patient care while ensuring no billable service is missed, supporting practice revenue growth and long-term sustainability.
Emerging Strategies: Technology and Patient Engagement

Modern tools enhance both revenue and patient satisfaction.
Examples:
- Telehealth reduces missed visits and expands patient access.
- Patient portals simplify bill payments and appointment scheduling.
- Automated engagement systems send reminders, wellness tips, and personalized messages to improve retention.
Investing in technology strengthens patient loyalty and ensures consistent revenue streams while reducing staff workload.
Medical Practice Revenue by Specialty
Every type of medical practice makes money differently. A family doctor’s office runs very differently from a surgery center or a specialist clinic. Understanding how revenue works in your specific specialty is the first step toward growing it effectively.
Primary Care and Family Practice
Primary care clinics see a high volume of patients but typically earn less per visit than specialists. The biggest revenue opportunities here come from keeping patients coming back regularly, offering preventive care services, and managing chronic conditions like diabetes or high blood pressure over the long term.
Key revenue drivers:
- Annual wellness visits and preventive screenings
- Chronic care management programs
- Vaccination and immunization services
- Telehealth follow-up appointments
- Lab testing performed in-house
Common revenue challenges:
- Lower reimbursement rates per visit
- High no-show rates affecting daily revenue
- Heavy administrative burden on front-desk staff
Specialist Clinics
Specialist practices earn more per visit than primary care but rely heavily on a steady stream of referrals to keep patient volume consistent. Missing even a small number of referrals or losing a referring physician relationship can have a big impact on monthly revenue.
Key revenue drivers:
- Procedure-based services with higher reimbursement rates
- Strong referral network management
- Diagnostic services performed in-house
- Bundled service packages for common conditions
Common revenue challenges:
- Heavy dependence on referral relationships
- Complex prior authorization requirements
- Higher claim denial rates due to procedure complexity
Surgical Practices
Surgical practices generate the highest revenue per patient encounter but also carry the highest operational costs. Getting paid correctly for surgical procedures requires precise coding, thorough documentation, and strong payer contract negotiation skills.
Key revenue drivers:
- High-value surgical procedures
- Anesthesia and facility fee billing
- Post-operative follow-up care
- Implant and device billing
Common revenue challenges:
- Complex coding requirements increase denial risk
- Long accounts receivable cycles
- High overhead costs reduce net profit margins
Pediatric Practices
Pediatric clinics serve younger patients and their families, with revenue tied closely to well-child visits, vaccinations, and acute care appointments. Seasonal demand spikes during flu season and back-to-school periods create both revenue opportunities and scheduling challenges.
Key revenue drivers:
- Well-child visits and developmental screenings
- Vaccination programs
- Acute illness appointments
- Behavioral health add-on services
Common revenue challenges:
- Lower reimbursement rates from Medicaid-heavy payer mix
- Seasonal revenue fluctuations
- High appointment volume required to maintain profitability
Mental Health and Behavioral Health Practices
Mental health practices have seen significant growth in demand but face unique billing challenges. Sessions are time-based, reimbursement rates vary widely by payer, and no-show rates tend to be higher than in other specialties.
Key revenue drivers:
- Individual and group therapy sessions
- Telehealth appointments expanding patient access
- Psychiatric medication management visits
- Employee assistance program contracts
Common revenue challenges:
- Inconsistent payer reimbursement for behavioral health services
- Higher no-show rates reducing daily revenue
- Limited billing codes compared to procedure-based specialties
Quick Comparison by Specialty
| Specialty | Average Revenue Per Visit | Biggest Revenue Driver | Biggest Revenue Challenge |
|---|---|---|---|
| Primary Care | $150 to $250 | Preventive and chronic care | Low reimbursement per visit |
| Specialist | $200 to $600 | Procedures and referrals | Prior authorization delays |
| Surgical | $500 and above | Surgical procedures | Complex coding and denials |
| Pediatric | $100 to $200 | Well-child and vaccination visits | Medicaid payer mix |
| Mental Health | $100 to $250 | Therapy sessions and telehealth | High no-show rates |
No matter what specialty you practice in, the path to stronger revenue runs through the same core habits: accurate billing, consistent patient retention, smart use of technology, and a clear understanding of where your money is coming from and where it is being lost.
How Small and Mid-Size Practices Can Increase Revenue Without Burnout
Small and mid-size clinics can grow revenue without overburdening staff by:
- Using efficient scheduling and delegation tools.
- Prioritizing high-impact initiatives.
- Aligning revenue strategies with operational capacity.
Well-trained staff, clear processes, and supportive technology enable sustainable growth, improved practice profitability, and better patient care.
Mistakes to Avoid When Trying to Increase Revenue
- Focusing only on volume: Seeing more patients doesn’t guarantee revenue growth without efficient processes.
- Neglecting patient experience: Poor communication and long wait times hurt retention.
- Overlooking billing fundamentals: Missed charges or unaddressed denials cost money.
- Implementing too many changes at once: Staff may become overwhelmed, creating inefficiencies.
Avoiding these mistakes with the help of healthcare IT solutions ensures sustainable revenue growth over time.
How to Get Started With Revenue Improvement
Improving your revenue begins with a deep dive into your current operations. By understanding where losses are occurring, you can create strategies to plug those gaps and maximize your earnings.
Step 1: Identify Revenue Leaks
Audit workflows, billing, and operations to uncover opportunities for improvement.
Step 2: Prioritize High-Impact Changes
Focus on initiatives that deliver the biggest financial return, such as reducing appointment no-shows or improving billing efficiency.
Step 3: Measure and Adjust
Track key metrics, including collections, denials, and patient retention, and refine strategies accordingly.
Conclusion
Increasing medical practice revenue is about working smarter, not harder. By implementing the proven ways to increase medical practice revenue discussed above, clinics can strengthen financial health while maintaining high-quality care.
Gradual implementation of these strategies ensures sustainable growth, stronger practice profitability, and improved cash flow. Clinic leaders who prioritize patient-centered care alongside operational efficiency are well-positioned for long-term success in a competitive healthcare environment.
FAQs
What are the most effective ways to increase medical practice revenue?
Focus on reducing no-shows, improving patient retention, optimizing billing, increasing revenue per visit, and offering high-margin services.
How can small practices boost revenue without overworking staff?
Use automation, efficient scheduling, delegate tasks, and prioritize high-impact changes for sustainable growth.
What is the average revenue per patient visit?
The average revenue per patient visit typically ranges between $150 and $300 for primary care practices and $200 to $600 for specialist visits, varying by specialty, payer mix, and location.
What is a good collection rate for a medical practice?
A good collection rate for a medical practice is generally 95% or higher, meaning you are successfully collecting 95 cents or more for every dollar owed after adjustments and write-offs.
Can technology help increase practice revenue?
Yes. Tools like automated reminders, telehealth, patient portals, and billing systems improve efficiency and collections.
How do I reduce claim denial rates in my practice?
Reduce denials by tightening front‑end work: verify eligibility and prior authorization before every visit, keep patient data accurate, and submit clean, well‑documented, correctly coded claims on time.
How does prior authorization affect medical practice revenue?
Prior authorization can slow cash flow, increase write‑offs, and add thousands in administrative costs per physician each year, so unmanaged PA quickly becomes a major bottleneck in your revenue cycle.
Stop Leaving Revenue on the Table
Book a call to see how MedLaunch’s AI-driven tools eliminate billing gaps, slash no-show rates, and recover lost revenue so you can grow.