Key Takeaways
-
1Patient activation defined: Activated patients understand their condition, feel confident managing it, and take proactive ownership of their health between visits.
-
2PAM levels differ: Each Patient Activation Measure level requires different support; using the same approach for all patients wastes resources and limits outcomes.
-
3Trust enables activation: Patients who trust their provider are more likely to follow guidance and stay engaged in their care plans.
-
4Shared decisions work: Patients involved in choosing their treatment plans are far more likely to follow them than those simply given instructions.
-
5Activation data guides care: PAM scores and patient feedback should shape follow-ups, education, and care coordination for each patient.
Patient activation has emerged as one of the most critical components in modern healthcare. Engaged and proactive patients not only experience better health outcomes but also help clinics operate more efficiently.
Understanding, measuring, and improving patient activation can transform how care is delivered, ensuring that patients are not just passive recipients of healthcare but active participants in their wellness journey.
Table of Contents
What is Patient Activation?
Patient activation refers to the knowledge, skills, confidence, and willingness of patients to manage their own health and healthcare. Activated patients understand their conditions, follow treatment plans, communicate effectively with providers, and take proactive steps toward better health.
Patient activation in healthcare is a multidimensional concept. It’s not simply about showing up to appointments, it’s about patient autonomy, self-management, and proactive participation in their health journey.
Patient Activation vs Patient Engagement

While often used interchangeably, patient activation and patient engagement differ:
| Aspect | Patient Activation | Patient Engagement |
| Definition | A patient’s knowledge, skills, confidence, and ability to manage their health | A patient’s behavioral and emotional involvement in healthcare processes |
| Focus | Individual readiness and autonomy | Interaction between patient and healthcare system |
| Example | Taking medication as prescribed, monitoring symptoms | Attending appointments, using patient portals |
In short, patient engagement focuses on the interaction, while patient activation focuses on the capability and confidence of the patient to act independently.
Why is Patient Activation Important?
Research shows that activated patients achieve better health outcomes and lower healthcare costs. According to the Agency for Healthcare Research and Quality (AHRQ):
- Patients with higher activation levels are 38% more likely to adhere to treatment plans.
- 30% fewer hospitalizations occur among highly activated patients.
- Clinics that invest in activation strategies see a 21% improvement in patient satisfaction scores.
Table 1: Impact of Patient Activation on Health Outcomes
| Activation Level | Treatment Adherence | Risk of Hospitalization | Patient Satisfaction |
| Low | 25% | High | Moderate |
| Medium | 50% | Moderate | Good |
| High | 85% | Low | Excellent |
Clearly, improving patient activation is not just beneficial—it’s essential for sustainable healthcare delivery.
Levels of Patient Activation (PAM)
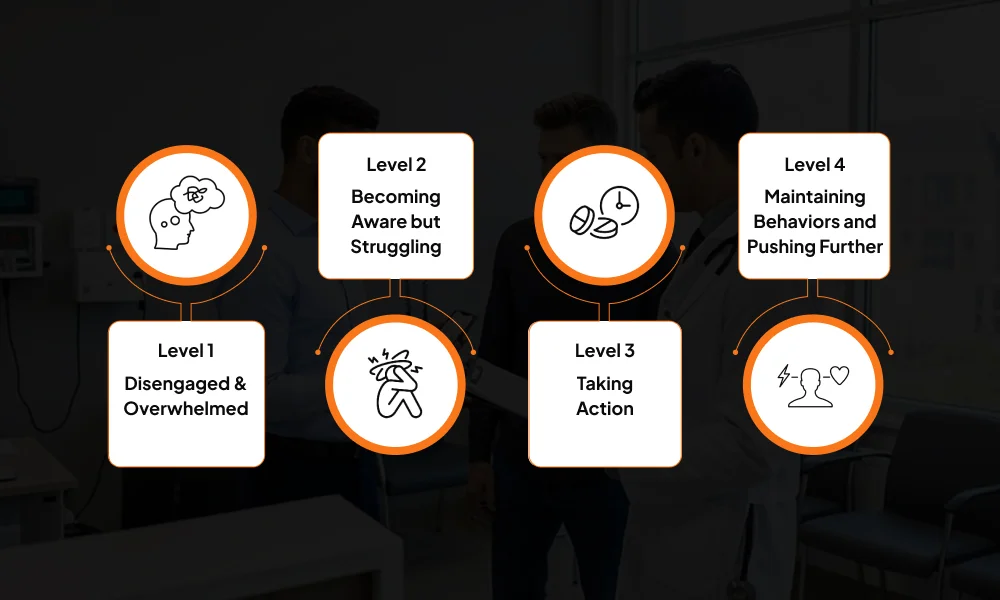
Overview of the Patient Activation Measure (PAM)
The Patient Activation Measure (PAM) is a validated tool used to assess a patient’s level of activation. It evaluates knowledge, skills, and confidence in managing health and provides a framework to tailor interventions.
Understanding the Different Levels of Activation
PAM categorizes patients into four levels:
- Level 1 – Disengaged and Overwhelmed: Patients are passive, do not see their health as their responsibility.
- Level 2 – Becoming Aware but Struggling: Patients know they need to act but lack confidence.
- Level 3 – Taking Action: Patients actively follow care plans and monitor their health.
- Level 4 – Maintaining Behaviors and Pushing Further: Patients consistently manage health proactively and are prepared for challenges.
Tailoring care strategies to these levels is crucial for maximizing patient activation.
Key Aspects of Patient Activation
Awareness and Knowledge
Health literacy plays a major role. Patients need to understand their conditions, risks, and treatment options. Clinics can improve activation by providing easy-to-understand educational materials, workshops, and online resources.
Motivation and Confidence

Patients must feel capable of managing their health. Techniques like motivational interviewing help build confidence and empower patients to take control of their care.
Behavioral Changes and Self-management
High activation leads to sustained behavioral changes, such as adhering to medications, monitoring vital signs, exercising, and attending follow-ups—ultimately reducing complications and improving quality of life.
Benefits of High Activation
Improved Health Outcomes
Activated patients show better adherence to treatment plans, resulting in fewer complications and better management of chronic diseases like diabetes, hypertension, and heart disease.
Better Patient Satisfaction
Patients who feel involved in decision-making and understand their health journey report higher satisfaction scores, building trust and long-term loyalty with the clinic.
Reduced Healthcare Costs
Clinics see reduced emergency visits, hospitalizations, and readmissions when patients take an active role in self-management, ultimately optimizing patient flow and activation.
Common Barriers and Mistakes in Patient Activation

Barriers to Patient Activation
- Low health literacy
- Lack of motivation or confidence
- Cultural or language differences
- Limited access to technology or support
Common Mistakes Healthcare Providers Make
- Assuming patients understand instructions
- Using one-size-fits-all care plans
- Focusing only on treatment, not education
- Neglecting follow-ups and reminders
How to Overcome These Challenges
- Provide personalized education materials
- Use patient activation management tools to tailor interventions
- Incorporate technology and reminders
- Foster an inclusive and supportive environment
10 Patient Activation Strategies Every Clinic Should Use
Strategy 1: Assess Every Patient’s Activation Level
Activation strategies that are not matched to a patient’s current level produce poor results. A Level 1 patient, someone who is passive, overwhelmed, and does not yet see their health as their responsibility, needs fundamentally different support than a Level 4 patient who is already managing their condition proactively and needs challenges rather than basic guidance.
The Patient Activation Measure (PAM) is a validated 13-question survey that takes under five minutes to complete and assigns patients to one of four levels. Administer it at the first visit, or include it as part of your new patient intake form. The score does not go into the chart as a diagnosis — it goes to the care team as a care planning signal.
In practice, this means your care plan templates should have four variants for any condition you manage frequently. A Level 1 diabetic patient gets a simplified one-page action plan with one goal and a scheduled follow-up call in one week.
A Level 4 diabetic patient gets a detailed self-monitoring protocol, access to advanced educational resources, and a quarterly review. Using the same care plan for both wastes one patient’s time and overwhelms the other.
Strategy 2: Build Trust Through Consistency
Trust is the precondition for activation. A patient who does not trust their provider will not follow care plans, will not disclose barriers to adherence, and will not return after a difficult interaction. Trust in a clinical setting is built differently than many providers assume. It comes primarily from consistency and reliability, not from warmth alone.
Consistency means the same provider sees the same patient whenever possible. It means promised follow-up calls happen when they were promised to happen. It means care instructions given verbally match what appears in the written summary. It means billing statements are clear and match what the patient was told to expect.
Audit your current processes for consistency failures. If patients are regularly seen by different providers at each visit with no handoff briefing, that is a trust erosion point. If follow up calls are scheduled but frequently missed or delayed, that is also a trust erosion point. Fix the process before focusing on communication style. Patients experience reliability before they experience warmth.
Strategy 3: Use Shared Decision-Making as a Structured Practice
Shared decision making is often treated as a tone shift, speaking more collaboratively and using open ended questions. That interpretation is too limited to produce the activation gains that research has documented.
Structured shared decision making means three specific things happen in every care conversation where a decision is being made. First, the provider presents the realistic options, including watchful waiting when appropriate, with honest descriptions of the likely outcomes for each.
Second, the patient’s priorities, constraints, and preferences are explicitly asked about rather than assumed. Third, the chosen plan is summarized back to the patient and confirmed as something they are willing and able to follow.
The third step is where most practices fall short. A provider may present options and ask questions but still write a plan based on clinical preference rather than the patient’s stated capacity. A patient who leaves with a plan they did not truly agree to, or agreed to only to avoid conflict, is unlikely to follow it.
At the end of every care conversation involving a treatment decision, ask directly, “Is there anything about this plan that would be difficult for you to follow?” That question alone can improve adherence because it gives patients permission to identify real barriers before they leave.
Strategy 4: Set Goals That Are Specific, Near-Term, and Patient-Selected

Generic goal setting such as “exercise more,” “eat better,” or “reduce stress” produces no measurable change in activation. Goals work when they are specific enough to be observable, near term enough to feel achievable, and chosen by the patient rather than assigned by the provider.
A useful goal for a sedentary patient with hypertension is not “increase physical activity.” It is “walk for 15 minutes after dinner on Monday, Wednesday, and Friday for the next three weeks.” The patient selected this specific activity from a short menu of options the provider offered. There is a defined review point — three weeks — and a single behavior change, not a lifestyle overhaul.
In practice, this means your clinical staff needs a brief goal-setting protocol. At the end of each visit where a behavior change is relevant, the provider or health coach spends three minutes with the patient identifying one specific action, its frequency, and its duration.
This is written down and given to the patient. At the next visit, the first question is about that specific goal — not general wellness, not the full care plan, just the one thing the patient committed to. This follow-through signals that the goal mattered and builds the accountability structure that makes future goals credible.
Strategy 5: Personalize Education to Health Literacy Level and Format Preference
Patient education that patients cannot understand or will not engage with does not activate anyone. The problem in most practices is that education materials are written at a reading level significantly higher than the average patient’s functional health literacy, and they are delivered in a single format regardless of what the patient would actually find useful.
Fix both problems separately. For reading level: audit your most frequently distributed patient education materials and rewrite any that assume more than a sixth-grade reading level.
Use short sentences, plain language, and specific instructions rather than general principles. Replace “monitor your glucose levels regularly” with “check your blood sugar every morning before breakfast and write the number in your log.”
For format: ask patients directly how they prefer to receive health information — reading, watching, listening, or talking through it with a staff member. Keep a simple note in each patient’s chart. A patient who retains information from short videos should receive video links in their follow-up message, not a PDF handout.
A patient who prefers to talk things through should have their education delivered conversationally during the visit, not handed a pamphlet at check-out. Neither approach costs more — it just requires recording the preference and acting on it consistently.
Strategy 6: Structure Follow-Up Around Accountability, Not Just Information
The purpose of a follow-up call or message is widely misunderstood. Most follow-up in clinical practice is informational — sending lab results, confirming appointments, sharing educational materials. Information delivery is necessary but not sufficient for activation.
Activating follow-up is accountability follow-up. It references the specific goal the patient set at their last visit, asks what happened, responds to what actually happened rather than what was supposed to happen, and sets the next small step.
Design a follow-up protocol for your highest-priority patient populations — typically patients managing chronic conditions or recently discharged. The protocol should specify who makes the contact (provider, nurse, health coach, or care coordinator), when it happens (days after visit, not weeks), what questions are asked, and what happens if the patient is not progressing. A ten-minute structured follow-up call within 48 hours of a visit produces more activation movement than a detailed care plan mailed two weeks later.
For patients who need more frequent touchpoints than staff capacity can support through calls, structured text check-ins — short, specific, two-way messages that ask one question and allow one response — maintain the accountability thread between visits without consuming clinical time.
Strategy 7: Apply Motivational Interviewing at the Moments That Matter
Motivational interviewing is most useful at specific inflection points — not as a general conversational style applied to every interaction, but as a structured technique deployed when a patient expresses ambivalence, resistance, or low confidence about a behavior change.
The four core techniques are open-ended questions, affirmations, reflective listening, and summaries (OARS). In clinical practice, the most impactful of these is reflective listening — paraphrasing what the patient said in a way that demonstrates understanding before responding.
A patient who says “I know I should check my blood sugar but I always forget” is expressing a behavior problem, not a knowledge problem.
A provider who responds with more information about why glucose monitoring matters has not listened. A provider who reflects “it sounds like remembering to fit it into your routine is the main challenge” has opened the conversation toward a practical solution.
Train clinical staff in OARS through scenario-based role play, not lecture. A two-hour workshop with four to five realistic patient scenarios produces more lasting behavior change in providers than a full-day training without practice.
Revisit the technique in monthly team huddles with one case example. The goal is for these responses to become reflexive at the moments that most determine whether a patient leaves more activated or less.
Strategy 8: Use Incentives Tied to Process Behaviors, Not Just Outcomes
Incentive programs for patient activation work when they reward actions the patient controls, not health outcomes they may not fully control. Rewarding a patient for lowering their A1c by two points over three months sounds sensible but punishes a patient who followed their care plan perfectly and still did not hit the number due to factors outside their control. That patient leaves less motivated, not more.
Effective incentive design rewards showing up — completing educational sessions, attending scheduled follow-ups, submitting home monitoring logs, completing their PAM assessment, or using the patient portal to message their care team. These are all behaviors entirely within the patient’s control and all of them are directly correlated with improved activation.
Keep incentives modest and immediate. A small reward — a reduced co-pay, a pharmacy discount, a tangible acknowledgment — given within days of the behavior is more activating than a large reward promised at the end of a long program. The behavioral principle is reinforcement proximity: the closer in time the reward follows the behavior, the stronger the association.
Strategy 9: Build a Collaborative Care Team With Defined Activation Roles

No single role in a clinic can carry full responsibility for patient activation. Providers have limited visit time. Nurses have clinical priorities. Front desk staff have administrative demands. Activation breaks down when it is assumed that someone else is handling it.
Define activation responsibilities explicitly by role. The provider’s activation role is diagnosis, goal-setting, and shared decision-making during the visit. The nurse or medical assistant’s activation role is pre-visit education, post-visit reinforcement, and flagging patients who are not progressing.
A health coach or care coordinator, where the practice has one, carries the longitudinal relationship — the consistent touchpoint between visits that tracks progress and adjusts the plan.
The front desk’s activation role is framing — how appointments are confirmed, how patients are welcomed, and whether the experience of arriving signals that the practice is organized and the patient’s time is valued.
Write these roles into your job descriptions and review them in onboarding. When every team member knows their specific activation contribution and sees how it connects to the others, accountability becomes structural rather than aspirational.
Strategy 10: Measure Activation Longitudinally and Use the Data to Adjust Care Plans

Measuring activation once, at intake, tells you where a patient started. Measuring it at each visit tells you whether your interventions are working — and for which patients they are working most. Without longitudinal PAM data, you are operating a program you cannot evaluate.
Set a measurement cadence based on patient type. For patients managing chronic conditions, administer the PAM every three to six months. For post-discharge patients, administer it at the two-week follow-up visit and again at three months. For new patients, administer at intake and at the six-month mark.
Use the data at two levels. At the individual level, a PAM score that has not moved after two measurement cycles signals that the current approach is not working for that patient — try a different format, a different goal type, or a different follow-up structure.
At the practice level, aggregate PAM scores by condition, by provider, and by care team tell you where activation programs are succeeding and where they are not. A provider whose panel shows consistently lower average activation than peers is not necessarily underperforming — they may have a higher-complexity patient population — but that signal warrants a conversation about whether additional support resources are needed.
Activation data should be reviewed in monthly team meetings alongside clinical outcomes. The question is not just “are our patients healthier” but “are our patients becoming more capable of managing their health.” Those are related but distinct, and both deserve a metric on your dashboard.
Conclusion
Improving patient activation is not just a theoretical concept; it has measurable impacts on health outcomes, patient satisfaction, and clinic efficiency.
Use Case Example: A primary care clinic implemented a 10-step patient activation strategy, including personalized care plans, regular follow-ups, and patient education workshops. Within six months, hospital readmissions decreased by 25%, and patient satisfaction scores rose from 78% to 92%. Patients reported feeling more confident and engaged in their care.
By systematically implementing patient activation strategies, clinics can empower patients, reduce costs, and foster a healthcare system that works for both providers and patients.
FAQs
What is patient activation in healthcare?
Patient activation refers to a patient’s knowledge, confidence, and skills to manage their own health and make informed healthcare decisions.
How is patient activation different from patient engagement?
Activation measures a patient’s ability and confidence to take charge of their health, while engagement focuses on the actions and interactions between patients and healthcare providers.
Why is patient activation important for clinics?
High patient activation leads to better health outcomes, improved patient satisfaction, and reduced healthcare costs.
How can clinics measure patient activation?
Clinics can use tools like the Patient Activation Measure (PAM) survey, health literacy assessments, and patient-reported outcome measures to track activation levels.
What are simple strategies to improve patient activation?
Strategies include personalizing care plans, encouraging self-management, setting achievable goals, regular follow-ups, patient education, and using technology like apps or reminders.




