Key Takeaways
-
1Redefine Workflows: Investing in queue software alone will not solve delays. Real improvement begins with redesigning workflows before implementing technology.
-
2Perceived Wait-Times: Patients often perceive wait times as 30 to 50% longer without updates. Clear communication through SMS, WhatsApp, or displays can reduce frustration.
-
3Visit Type: Separating queues by visit type such as labs, vaccinations, or follow-ups prevents simple cases from delaying more complex consultations.
-
4Effective Queues: Effective queue optimization requires people, clear processes, data insights, and supportive technology working together.
-
5Sustainable Changes: A phased approach to queue improvements delivers better results than a full overhaul, allowing gradual and sustainable operational changes.
Patient Queue Optimization is the structured process of redesigning how patients move through a clinic, from booking to check-in, consultation, diagnostics, billing, and follow-up, to reduce unnecessary waiting, improve communication, and maximize clinical efficiency.
Effective patient flow management ensures that every step from booking to discharge operates as a connected system rather than a series of isolated touchpoints.
In group practices and multi-provider clinics, patient queues directly influence three critical outcomes:
- Patient experience – Patient experience improvement begins with eliminating the uncertainty that makes waiting feel longer than it actually is.
- Revenue performance – Walkouts, no-shows, and inefficiencies quietly drain profitability.
- Clinician productivity – Poor flow leads to rushed consultations, idle time, or burnout.
Many organizations attempt to solve delays by purchasing queue software or installing kiosks. But real patient queue optimization goes far beyond installing tools. It involves redesigning workflows, defining ownership, aligning communication, and using data intelligently.
MedLaunch works with clinics and group practices not to “install another system,” but to redesign patient flow strategically. The focus is on sustainable operational improvement—where technology supports process, not the other way around.
Table of Contents
Why Patient Queue Management Matters More in Group Practices

Patient queue management in a single-provider clinic is relatively straightforward. In contrast, group practices often operate like mini health systems. Under one roof you may find:
- Primary care
- Specialty consults
- Diagnostics and imaging
- Lab services
- Pharmacy or dispensing
- Multiple providers with varying schedules
In multi-location networks, the complexity multiplies. Different specialties, appointment templates, walk-ins, shared staff, and resource constraints all interact dynamically.
This is precisely why outpatient flow optimization requires a fundamentally different approach than single-provider clinic management.
The Real Impact of Long Wait Times
In group settings, unmanaged queues can lead to:
- Walkouts: Patients leave without being seen after long waits.
- No-shows and cancellations: Poor prior experiences discourage future bookings.
- Negative online reviews: Wait time is one of the most cited complaints.
- Clinician burnout: Providers feel constantly behind schedule.
- Revenue leakage: Patients shift to competitors with more predictable service.
Multiple studies show that patients often spend more time waiting than they do with their clinician, with average waits commonly in the 20–40 minute range for visits that last 10–20 minutes.
In many clinics, this imbalance leaves front-desk teams fielding constant “How much longer?” calls and walk‑ups instead of focusing on higher‑value tasks.
Patient wait time reduction is therefore not just an operational goal but a direct driver of satisfaction scores, retention, and revenue stability.
For group practices, optimizing patient queues is not optional—it is operationally critical.
The Hidden Cost of Poor Patient Queues
When queues are unmanaged, the costs extend beyond visible wait times.
1. Lost Revenue
Walkouts and deferred care directly reduce daily billing. If even 3–5 patients leave daily in a mid-sized clinic, the annual impact can reach six figures.
2. Clinical Schedule Disruption
Long waits create overruns. Left unaddressed, these overruns compound into appointment backlogs that take days or weeks to clear, disrupting provider schedules and patient access simultaneously. Overruns lead to:
- Rushed consults
- Reduced quality interactions
- Provider stress
- Delays cascading into later appointments
Conversely, poor balancing can cause idle time, where providers sit waiting for patients due to bottlenecks upstream, turning underutilized clinical time into a silent but measurable revenue loss.
3. Operational Drag
Front-desk staff become overwhelmed with manual triage and constant updates. Nurses repeatedly explain delays. Physicians are interrupted mid-consult to address flow issues.
Poor patient queue management strategies create friction across every layer of the organization, quietly eroding the medical practice efficiency that sustains long-term growth.
Common Patient Queue Challenges in Medical Practices

Before implementing patient queue improvement initiatives, it’s essential to understand common challenges.
1. Unpredictable Walk-Ins vs Scheduled Patients
Walk-ins can disrupt tightly planned schedules. Without proper segmentation, urgent cases and routine visits compete for the same queue.
2. Peak Congestion
Many clinics experience consistent bottlenecks:
- Monday mornings
- Post-lunch surges
- Specific high-demand providers
- Seasonal spikes
Without analyzing arrival patterns, staff allocation remains reactive instead of proactive.
3. Bottlenecks at Key Touchpoints
Common choke points include:
- Registration
- Insurance verification
- Vitals collection
- Diagnostics
- Billing
Even if consultation rooms are available, patients can remain stuck in earlier steps.
4. Lack of Visibility Across Locations
In group practices, patients may move between departments. Without real-time patient queue tracking, individuals can get “lost” between steps, leading to repeated questioning and frustration.
Experience Gaps Patients Feel But You Don’t See
Often, operational leaders focus on measurable wait times—but perception is equally important.
Overestimation of Wait Time
Patients typically perceive waits as 30–50% longer than actual duration, especially without updates.
Anxiety from Uncertainty
Not knowing “what’s next” or “how much longer” increases stress. Uncertainty feels worse than waiting itself.
Inconsistent Communication
If front-desk staff say 15 minutes and nurses say 30, trust erodes. Even small inconsistencies damage perceived quality.
Optimizing patient queues must address both operational metrics and psychological experience.
Patient Queue Optimization vs. Queue Management Software

One of the most common misconceptions is equating software with optimization.
Software = Tools
- Token systems
- Kiosks
- Digital boards
- Mobile apps
Optimization = System Redesign
- Workflow standardization
- Triage rules
- Staff roles
- Communication protocols
- Data governance
Many clinics invest in a healthcare queue management system without first redesigning the processes that system is meant to support, leading to poor adoption and unchanged outcomes. Adoption falters. Staff revert to manual workarounds. KPIs remain misaligned.
True clinic patient queue optimization begins with understanding flow, then selecting supportive tools only when necessary.
MedLaunch positions itself as a solutions partner—plugging into existing systems, recommending technology strategically, and ensuring processes drive performance.
A Holistic Framework for Patient Queue Optimization
Sustainable clinic workflow optimization is not about a single fix. It requires four interconnected pillars working together to keep patient flow consistent, predictable, and scalable.
1. People
Queue management starts with the right people in the right roles. Staff need clear responsibilities for monitoring patient flow, the training to spot bottlenecks early, and the authority to act before delays affect patient experience. No system works without accountable, well-prepared people behind it.
2. Process
Standardized workflows remove the inconsistency that causes delays. When triage protocols, patient hand-offs, and departmental procedures are clearly defined and consistently followed, queues move predictably and staff spend less time making judgment calls under pressure.
3. Data
You cannot improve what you do not measure. Monitoring arrival patterns, wait times at each step, and no-show rates gives facility managers the insight to anticipate problems, allocate resources effectively, and make decisions based on evidence rather than intuition.
4. Technology
The right technology makes everything else easier. Automated scheduling, digital check-ins, and real-time queue dashboards reduce manual workload and give staff the visibility they need to manage flow without adding operational complexity.
This framework ensures outpatient patient queue optimization efforts remain practical and scalable.
Key Patient Queue Optimization Strategies
Strategy 1 – Map and Standardize the Patient Journey
Effective queue optimization begins with understanding exactly how patients move through your facility. Mapping the end-to-end flow by visit type, whether new or returning, walk-in or scheduled, urgent or routine, reveals where delays are built into the process rather than caused by them.
Every queue point from registration and triage to billing and pharmacy should be mapped and monitored as part of this process. Making each step visible allows clinics to identify bottlenecks and focus on improvements that reduce wait times and streamline patient movement.
Visit types to map:
- New patient vs. existing patient
- Walk-in vs. appointment
- Urgent vs. routine
- Diagnostic-only vs. consultation
Queue points to identify:
- Pharmacy.
- Registration
- Waiting area
- Triage
- Diagnostics
- Consultation
- Billing
Creating Standardized Pathways by Visit Type
Once the full journey is mapped, separate pathways should be designed for different visit categories:
| Visit Type | Examples |
|---|---|
| Quick Visits | Prescription refills, injections, lab follow-ups |
| Complex Visits | New consultations, multi-specialty evaluations |
Standardized pathways enable smarter batching, fair prioritization, and faster throughput without creating the perception of bias among waiting patients.
Strategy 2 – Segment and Prioritize Queues Intelligently
Treating every patient identically regardless of clinical urgency or visit complexity is one of the most common causes of unnecessary congestion.
Effective segmentation uses criteria such as clinical urgency, appointment type, provider availability, and resource dependency to route patients into appropriate queues from the moment they arrive, or even before, through digital intake forms and referral data.
When combined with triage optimization protocols, segmentation ensures the right patients reach the right providers at the right time.
Segmentation criteria:
- Resource dependency
- Clinical urgency
- Appointment type
- Provider schedule
Fast-Track Queues for Low-Complexity Visits
Dedicated fast-track queues for labs, vaccinations, and stable chronic follow-ups prevent simple cases from stacking behind complex ones.
This single change visibly improves flow perception for the majority of patients while protecting consultation time for those who genuinely need it.
Virtual queue systems can further decouple physical presence from processing sequence, allowing patients to be managed in order without occupying the same physical space.
Strategy 3 – Use Proactive Communication to Manage Expectations

Research consistently shows that perceived wait time is more damaging to patient satisfaction than actual wait time. When patients know where they are in the queue, what to expect next, and are notified promptly if delays occur, frustration drops significantly even when the wait itself remains unchanged.
A modern patient flow solution makes this level of transparency automatic by tracking each step of the visit, surfacing real‑time queue updates, and proactively communicating delays before patients need to ask.
Communication channels to use:
- Standardized front-desk scripts
- SMS and WhatsApp
- In-app notifications
- Digital display boards
What to Communicate and When
| Touchpoint | What to Communicate |
|---|---|
| At Booking | Visit duration, required documents, pre-visit forms |
| On Arrival | Check-in status, queue position, wait estimate |
| During Wait | Delay notifications, option to wait elsewhere |
| After Visit | Feedback prompt on wait experience |
Proactive communication transforms waiting from a source of frustration into a predictable, manageable experience.
Strategy 4 – Redesign Front-Desk Workflows Around Patient Flow
Front-desk staff are frequently pulled in too many directions at once, managing registration, insurance verification, incoming calls, data entry, and queue updates simultaneously. This multitasking creates inconsistency and slows down the very touchpoint that sets the tone for the entire patient experience.
Ways to Reduce Front-Desk Overload
- Pre-visit digital intake forms
- Automated queue management systems
- Self-service check-in kiosks
- AI medical receptionist for routine calls
Role Clarity and Ownership of the Queue
Every facility needs clear answers to three questions:
- Who monitors real-time queue status?
- Who escalates when delays exceed acceptable thresholds?
- Who communicates with waiting patients?
Without this clarity, bottlenecks go unaddressed not because staff lack capability but because no one feels individually responsible for acting on them.
Strategy 5 – Design Physical and Virtual Waiting Spaces
The waiting environment is an underutilized lever in queue optimization. Physical design and virtual waiting options work together to reduce both actual and perceived congestion.
Physical design considerations:
- Comfortable and adequate seating
- Zoning by visit type
- Clear directional signage
- Reduced overcrowding through capacity management
Virtual waiting options:
- Wait in car or nearby location
- Receive SMS or app notification when nearly called
- Remote check-in upon return
Making Waiting Feel Shorter and Less Stressful
Small investments in the waiting environment deliver outsized returns in satisfaction scores. Consider adding:
- Visible real-time queue progress indicators
- Wi-Fi and charging stations
- Educational or entertainment screens
- Water dispensers and refreshments
- Separate family and quiet zones
Strategy 6 – Leverage Data to Continuously Optimize Patient Queues
Facilities that consistently outperform on patient flow share one common habit: they measure everything and act on what they find.
Key metrics to track:
| Metric | What It Reveals |
|---|---|
| Average wait time per step | Where bottlenecks are forming |
| Arrival pattern distribution | When demand peaks occur |
| No-show rate | Scheduling and reminder effectiveness |
| Walkout rate | Tolerance threshold for wait times |
| Provider idle time | Underutilized capacity |
Turning Queue Data into Operational Decisions
Data becomes valuable only when it drives action:
- Monthly metric reviews → embed continuous improvement into governance
- Arrival patterns → adjust staffing during peak hours
- No-show rates → refine overbooking thresholds and reminder protocols
- Step-level wait times → guide room allocation and slot length decisions
Strategy 7 – Digital Tools That Support (Not Overcomplicate)
Technology is most effective when it removes friction rather than adding it. The goal is not to implement the most sophisticated system available but to deploy healthcare automation solutions that staff can adopt quickly and patients can use without assistance.
Recommended lightweight tools:
- Online pre-registration portals
- Smart scheduling systems
- Waitlist automation
- QR-based self check-in
- Real-time queue dashboards
- Automated patient messaging
Integrating With Existing Systems
A common barrier to technology adoption is the assumption that improvement requires replacing existing practice management or EHR systems entirely. In most cases it does not.
Lightweight integrations layered onto existing infrastructure consistently deliver faster ROI with far less operational disruption than full system replacements.
Staged enhancements are the more practical and sustainable starting point for most outpatient facilities.
Implementation Roadmap for Group Practices
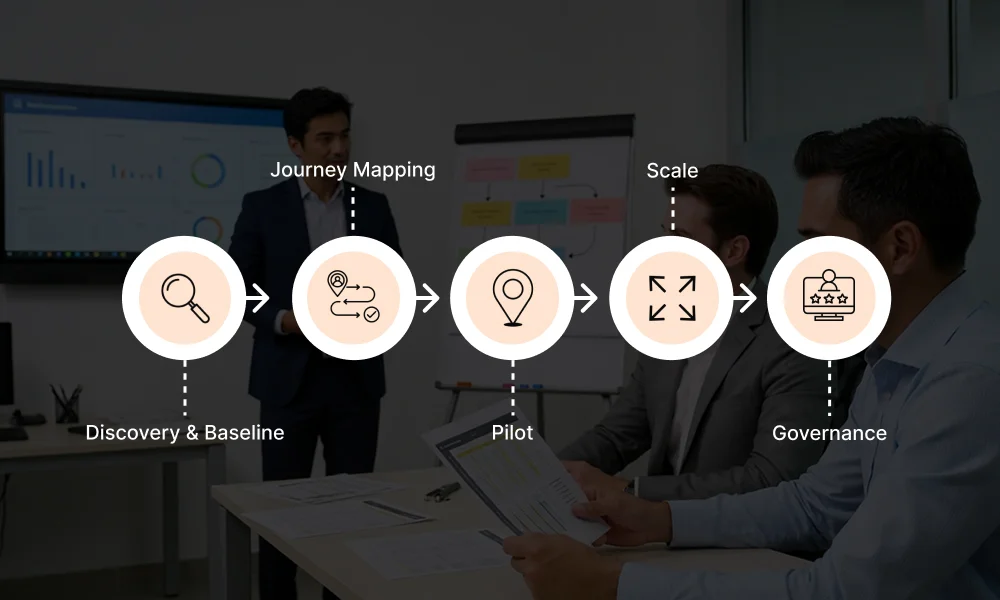
Optimizing patient queues across a group practice requires more than good intentions. Without a structured rollout plan, even well-designed changes risk creating temporary disruption that erodes staff confidence and patient trust. The following roadmap provides a phased approach that minimizes operational risk while building momentum at every stage.
Step 1 – Discovery and Baseline Measurement
Before any changes are made, a clear picture of current performance is essential. This stage is about gathering honest, data-driven insight into how the facility is operating today, not how it is assumed to be operating.
Metrics to measure at baseline:
| Metric | Why It Matters |
|---|---|
| Average wait time per step | Identifies where time is being lost in the patient journey |
| Walkout rate | Indicates the point at which patients lose tolerance for waiting |
| No-show rate | Reveals scheduling and communication gaps |
| Bottleneck locations | Pinpoints the specific queue points causing the most congestion |
| Staff utilization | Highlights imbalances between workload and capacity |
This baseline becomes the benchmark against which all future improvements are measured. Without it, there is no reliable way to know whether changes are working or simply shifting the problem elsewhere.
Step 2 – Journey Mapping and Opportunity Identification
With baseline data in hand, the next step is to map the full patient journey across every visit type and queue point. This exercise surfaces two categories of opportunity that should be prioritized differently.
Quick wins are changes that can be implemented immediately with minimal resource investment and that deliver visible improvement fast. Examples include introducing a dedicated queue for low-complexity visits, adding SMS wait time notifications, or clarifying front-desk role responsibilities. These early wins build staff confidence and demonstrate to leadership that the optimization effort is producing results.
High impact structural changes are deeper interventions that require more planning, investment, or cross departmental coordination. Examples include implementing digital pre registration or redesigning physical waiting areas to support smoother patient movement.
These improvements are usually prioritized for later stages and may include integrating real time queue dashboards with existing EHR systems. They are easier to implement once quick wins have helped establish organizational buy in.
Step 3 – Pilot in a Controlled Environment
Rather than rolling out changes facility-wide from the outset, piloting in a single specialty or location allows the team to test new workflows, identify unforeseen issues, and refine processes before broader implementation.
Choosing the right pilot site:
- Select a department with moderate patient volume, neither too quiet to generate meaningful data nor too busy to absorb the friction of change
- Choose a location where staff are open to process experimentation
- Ensure the pilot site has a designated lead responsible for monitoring outcomes and feeding back observations
During the pilot, track:
- Changes in wait times compared to baseline
- Staff adaptation and workflow friction points
- Patient feedback and satisfaction signals
- Any unintended consequences on adjacent departments
The pilot phase typically runs for four to eight weeks, long enough to capture meaningful performance data across varying demand conditions including peak and off-peak periods.
Step 4 – Scale Across Providers With Refined SOPs
Once the pilot has validated the approach and standard operating procedures have been refined based on real-world findings, the model is ready to be expanded across the broader practice.
Keys to successful scaling:
- Standardize without rigidity — SOPs should provide clear guidance while allowing department leads the flexibility to adapt to local nuances
- Train before you launch — every staff member affected by the new workflows should receive role-specific training before go-live, not during it
- Stagger the rollout — expanding one location or specialty at a time prevents organization-wide disruption and allows lessons from each rollout to inform the next
- Communicate with patients — inform patients of upcoming changes through booking confirmations, waiting area signage, and front-desk conversations to set accurate expectations
Step 5 – Embed Governance and Continuous Optimization
Queue optimization is not a project with a defined end date. It is an ongoing operational discipline that requires structured governance to sustain improvements over time and respond to evolving patient volumes, staffing changes, and service expansions.
Governance structure to implement:
- Monthly queue performance reviews with department leads using live metric dashboards
- Quarterly deep-dive audits comparing current performance against baseline and interim benchmarks
- A designated queue optimization lead or committee responsible for identifying emerging bottlenecks and coordinating responses
- A feedback loop between front-line staff and management so that operational issues are surfaced and addressed before they escalate
Facilities that embed this governance structure consistently outperform those that treat queue optimization as a one-time initiative, because they build the institutional habit of continuous improvement rather than relying on periodic interventions.
Example Scenario – From Chaotic to Predictable Queues
A mid-sized multi-specialty outpatient clinic serving approximately 300 patients per day was experiencing persistent operational challenges.
Walk-in lines regularly extended into corridors during peak morning hours, patient complaints about wait times were rising steadily, and staff were visibly overstretched managing competing administrative and patient-facing demands simultaneously.
The core problems were:
- A single undifferentiated queue handling all visit types regardless of complexity or urgency
- No digital intake process, meaning all registration was completed in person on arrival
- No real-time visibility into queue status for staff or patients
- Reactive staffing decisions made in response to congestion rather than in anticipation of it
- No structured communication to patients about expected wait times or delays
The cumulative effect was a facility where neither staff nor patients could predict how long anything would take, creating an environment of frustration, inefficiency, and eroding trust.
The Intervention
The clinic implemented a structured patient queue optimization program across a twelve-week period using the phased roadmap outlined above. Changes were introduced progressively rather than all at once to maintain operational stability throughout the transition.
Key changes implemented:
Segmented queues were introduced to separate low-complexity visits including labs, injections, and prescription refills from the main consultation queue. This immediately reduced congestion at the primary consultation desk and allowed straightforward cases to be processed in a fraction of the previous time.
Digital pre-registration was rolled out through the clinic’s patient portal, allowing patients to complete intake forms, submit insurance information, and verify personal details before arriving. Average in-person registration time dropped from fourteen minutes to under five minutes within the first month.
Proactive SMS communication was implemented to notify patients of their queue position, estimated wait time, and any delays beyond a fifteen-minute threshold. Patients were also given the option to wait in their vehicles and return when notified, reducing physical congestion in the waiting area significantly.
Data-driven staffing adjustments were made based on arrival pattern analysis from the baseline measurement phase. Additional registration and triage staff were scheduled during identified peak windows, reducing the bottleneck that had previously formed between 9am and 11am each weekday.
Real-time queue dashboards were installed at the front desk and nursing station, giving staff live visibility into queue length, step-level wait times, and emerging bottlenecks for the first time.
The Results
Within twelve weeks of full implementation the clinic recorded measurable improvements across every key performance metric established at baseline.
| Metric | Before | After |
|---|---|---|
| Average registration time | 14 minutes | 4.5 minutes |
| Average total wait time | 47 minutes | 28 minutes |
| Walkout rate | 11% | 3% |
| Patient satisfaction score | 3.2 / 5 | 4.6 / 5 |
| Peak hour congestion complaints | 34 per week | 6 per week |
Beyond the numbers, staff reported lower stress levels during peak periods, clearer role ownership, and greater confidence in their ability to manage patient flow proactively.
Provider schedules became more balanced as appointment slot lengths were refined using visit-type data, reducing the pattern of providers running significantly behind by mid-morning.
The clinic’s experience demonstrates that patient queue optimization does not require a complete operational overhaul.
A structured, phased approach focused on people, process, data, and the right technology produces compounding improvements that benefit patients, staff, and the facility’s reputation simultaneously.
Conclusion
Patient Queue Optimization is a strategic lever for growth in modern group practices. It reduces operational friction, enhances patient trust, and protects revenue.
Optimizing patient queues requires more than tools—it demands clarity in roles, standardization of process, intelligent segmentation, proactive communication, data-driven decisions, and thoughtful use of technology.
For clinics ready to move from reactive management to predictable performance, a structured approach to outpatient patient queue optimization can deliver measurable and sustainable impact.
MedLaunch partners with healthcare organizations to redesign patient flow systems that scale, without overwhelming teams or replacing core infrastructure.
If your clinic is experiencing long waits, walkouts, or operational stress, now is the time to rethink how your patient queues are designed.
A discovery audit focused on patient queue management could be the first step toward transforming your clinic’s operational performance.
FAQs
What are the best strategies to optimize patient queues?
Optimize patient queues by using smart scheduling, clear triage rules, digital or kiosk check-in, and real-time monitoring of wait times so staff can quickly rebalance patients and providers.
How do digital or virtual queue systems improve patient flow?
Digital or virtual queues let patients check in remotely, track their place in line, and receive updates, which reduces crowding, cuts perceived wait times, and keeps rooms and clinicians better utilized.
How can small practices implement low-cost queue improvements?
Small practices can tighten scheduling, use simple sign-in lists, add basic online booking and SMS reminders, and track daily wait times to spot and fix bottlenecks without expensive software.
How can SMS or WhatsApp notifications reduce waiting-room congestion?
SMS or WhatsApp alerts allow patients to wait elsewhere and return just before their turn, reducing waiting-room crowding and keeping the queue moving with fewer no-shows or missed calls.
What are common bottlenecks in patient queues and how to fix them?
Common bottlenecks include slow registration, unclear triage, and uneven provider availability; clinics can fix these with pre-registration, self-check-in, clear priority rules, and better alignment of staff schedules to demand.
Stop Losing Patients to Long Wait Times
Book a call to see how MedLaunch optimizes your patient flow, reduces walkouts, and uses AI to keep your clinic running on schedule around the clock.