Key Takeaways
-
1Journey optimization defined: Patient journey optimization maps care stages, identifies friction, and improves touchpoints across the patient experience.
-
2Friction compounds quickly: Difficult booking, long waits, unclear instructions, and missing follow-ups together create frustration that drives patients away.
-
3Cross-functional mapping: Effective journey mapping requires input from front desk, clinical, IT, and operations teams to capture the full patient experience.
-
4Start with one journey: Focus first on a high-impact journey like onboarding or follow-up to create measurable improvements before scaling changes.
-
5Continuous optimization: Patient journey optimization is ongoing; processes and expectations evolve, so journeys must be regularly reviewed and improved.
Healthcare today is no longer judged only by clinical outcomes. Patients evaluate their care based on how easy it is to book an appointment, how clearly they receive information, how long they wait, and how supported they feel after the visit. All of these moments together form the patient journey.
When that journey feels confusing, fragmented, or stressful, patients disengage, miss appointments, or seek care elsewhere. This is why Patient Journey Optimization has become a critical focus for healthcare organizations that want to improve access, satisfaction, outcomes, and long-term loyalty.
In this guide, we’ll explain what patient journey optimization really means, how it differs from patient experience, and how to systematically improve the patient journey in healthcare using mapping, data, design, and technology.
Table of Contents
What Is Patient Journey Optimization?

The patient journey refers to the complete, end-to-end experience a patient has with a healthcare organization. It starts long before the first appointment and continues well after the visit is over.
A typical patient journey may include:
- Becoming aware of a clinic or provider
- Researching options online
- Booking an appointment
- Preparing for the visit
- Receiving care
- Following up after the visit
- Continuing long-term care or building loyalty
Patient Journey Optimization is the process of intentionally improving each of these steps. It focuses on identifying friction points, closing gaps between departments, and designing smoother transitions across all touchpoints and channels.
Rather than treating issues in isolation, patient journey optimization looks at how every step connects. The goal is to reduce friction, improve clarity, and create a more consistent, supportive patient experience while also improving operational efficiency and outcomes.
Understanding the Patient Journey
To optimize the patient journey, it’s important to understand how patients actually move through the system and where problems typically arise.
Stages of the Patient Journey
While journeys vary by specialty and care type, most healthcare journeys include 5–6 core stages.
1. Awareness
The patient becomes aware of a healthcare provider through search engines, referrals, ads, or word of mouth.
- Patient action: Searches symptoms or providers online, reads reviews.
- Clinic action: Provides accurate information on the website, listings, and profiles.
2. Research and Consideration
The patient compares options and decides where to seek care.
- Patient action: Reviews services, insurance acceptance, availability, and reputation.
- Clinic action: Offers clear service descriptions, transparent pricing guidance, and trust signals.
3. Access and Booking
The patient tries to schedule an appointment.
- Patient action: Calls the clinic or uses online booking.
- Clinic action: Manages phone lines, online booking tools, and appointment availability.
4. Pre-Visit
The patient prepares for the visit.
- Patient action: Completes forms, reviews instructions, confirms appointment.
- Clinic action: Sends reminders, digital intake forms, and preparation instructions.
5. In-Visit
The patient arrives and receives care.
- Patient action: Checks in, waits, meets the care team, receives treatment.
- Clinic action: Manages check-in, rooming, clinical workflows, and communication.
6. Post-Visit and Follow-Up
The relationship continues after the visit.
- Patient action: Reviews instructions, completes follow-ups, pays bills, accesses results.
- Clinic action: Sends summaries, follow-up messages, billing statements, and care reminders.
Each stage includes multiple patient journey touchpoints that shape how patients perceive the entire experience.
Key Touchpoints Across the Journey
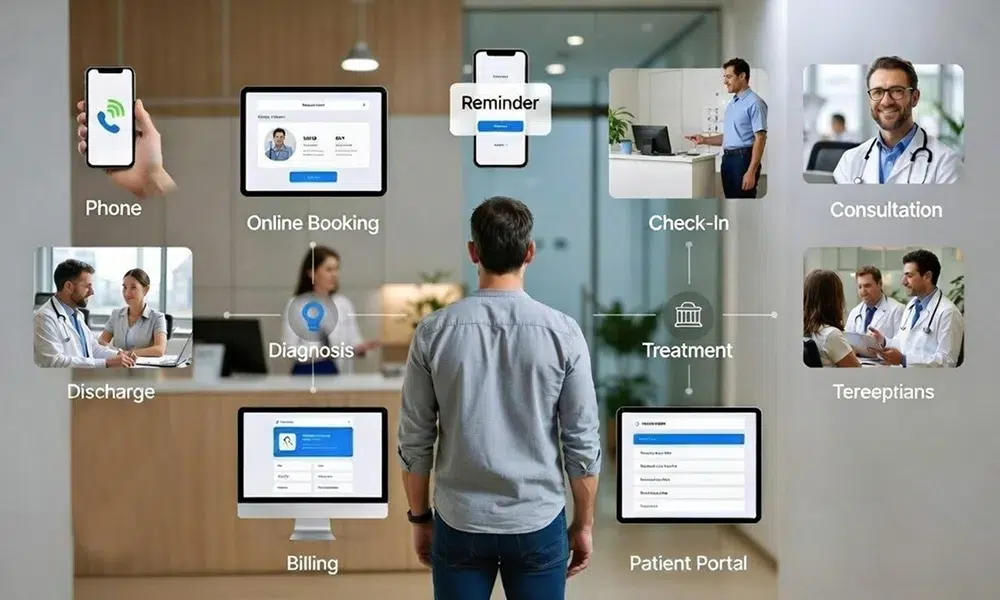
Patient journeys unfold across many touchpoints and channels, both digital and in-person.
Common touchpoints include:
- Website and search results
- Online reviews and provider profiles
- Phone calls and call center interactions
- Online booking and scheduling tools
- Appointment reminders and confirmations
- Check-in and waiting room experience
- Clinical encounter and provider communication
- Discharge instructions and education
- Billing statements and insurance communication
- Patient portal access
- Follow-up calls, messages, or surveys
Friction often appears when:
- Booking is difficult or requires long phone waits
- Instructions are unclear or inconsistent
- Wait times are unpredictable
- Bills are confusing or unexpected
- Follow-up communication is delayed or missing
Patient journey optimization focuses on smoothing these touchpoints and ensuring they connect logically across the end-to-end patient journey.
Patient Journey Optimization vs Patient Experience
Patient experience and patient journey optimization are closely related but not the same.
Patient experience refers to how patients feel about their care. It includes perceptions, emotions, trust, and satisfaction.
Patient journey optimization, on the other hand, is the structured process used to improve that experience. It involves mapping the journey, measuring performance at each stage, identifying pain points, and redesigning workflows and touchpoints.
In simple terms:
- Patient experience is the outcome
- Patient journey optimization is the method
Organizations that want to improve the patient journey in healthcare must go beyond friendliness and focus on systems, processes, and design that consistently support patients at every step.
Why Optimize the Patient Journey?

Optimizing the patient journey delivers value across clinical, operational, and financial dimensions.
- Better access and fewer barriers to care
Simplified booking and clear instructions reduce no-show rates and missed appointments. - Higher satisfaction and trust
Clear communication and smooth transitions reduce anxiety and build confidence. - Improved clinical outcomes
Better follow-up and adherence reduce errors and support better health outcomes. - Operational efficiency
Fewer calls, less rework, and smoother handoffs reduce staff burden. - Stronger retention and revenue
Patients who have positive journeys are more likely to return and recommend care.
Optimizing the patient journey across all touchpoints benefits both patients and care teams.
Key Components of Patient Journey Optimization
Successful patient journey optimization relies on four main components. Mapping, Feedback, Personalization, and Measurement.
Journey Mapping
Patient journey mapping involves visually documenting each step of the journey, including patient actions, emotions, touchpoints, and friction points. Maps are often created for priority journeys such as new patients, chronic care patients, or surgical pathways.
Feedback Collection

Patient feedback validates the journey map and reveals blind spots. Common methods include surveys, NPS scores, reviews, and interviews collected at key journey stages.
Personalization and Segmentation
Not all patients have the same needs. Segmenting patients (new vs existing, chronic vs acute, digitally comfortable vs not) allows clinics to tailor communication, reminders, and support.
Measurement and KPIs
Optimization requires measurement. Common metrics include:
- Time to next available appointment
- Digital booking rate
- Wait times
- Satisfaction scores
- Patient portal adoption
- Follow-up completion rates
These KPIs show where patients struggle and where improvements have the biggest impact.
The Role of Technology
Technology plays a central role in modern patient journey optimization, especially for digital patient journey optimization.
Key tools include:
- Online booking and self-scheduling
- Digital intake forms and check-in
- Patient portals for results and communication
- Automated reminders and follow-ups
- Two-way messaging and educational content
- Patient engagement platforms or CRMs
- Analytics dashboards to identify drop-offs and bottlenecks
Technology helps scale consistency, but it must be balanced with human support. Automation should remove friction, not make patients feel disconnected or ignored.
Steps to Implement Patient Journey Optimization

Patient journey optimization works best when implemented systematically. The steps below are written for a practice manager who is starting from scratch — someone who knows their current journey has problems but hasn’t yet begun the process of fixing them formally.
1. Choose a Priority Journey
Before mapping anything, decide which journey you are optimizing first. Trying to improve every patient journey simultaneously produces unfocused effort and inconclusive results. One journey, done properly, teaches you the method and delivers visible improvement you can build on.
How to choose: Look at where friction currently costs you the most. Ask three questions:
- Where do patients complain most often? Check your reviews, your front desk call log, and your patient satisfaction comments from the last three months. Recurring themes point to the journey that most needs attention.
- Where does staff time disappear? If your front desk spends two hours every morning re-entering intake data, or your nurses spend the first ten minutes of every visit re-collecting information patients already gave at booking, that journey is a priority candidate.
- Where is volume highest? The journey that affects the most patients every week has the highest return on improvement. For most practices, that is new patient onboarding.
Choose one. Write it down as a specific statement: not “new patients” but “the experience a patient has from their first contact with the practice through the end of their first visit.” That specificity keeps the project scoped and measurable.
2. Map the Current Journey
A journey map is a written, step-by-step account of exactly what happens today — not what is supposed to happen, and not what you would like to happen. Its purpose is to make the real workflow visible so that problems can be located precisely rather than described vaguely.
Who needs to be in the room: Bring together the people who actually perform each step of the journey. For new patient onboarding, that means at minimum one front desk staff member, one nurse or medical assistant, and one provider.
If your practice has a billing coordinator involved in insurance verification before the visit, include them. Do not map the journey with managers alone — managers know the policy; frontline staff know what actually happens.
How to run the mapping session: Give the group a blank wall or a shared document and work through the journey chronologically. For each step, record four things:
- What happens: the specific action taken, by whom, and using what tool or method
- What the patient experiences: what they see, receive, or are asked to do at this point
- How long it takes: an honest estimate, not an ideal
- What can go wrong: the failure modes your team has seen at this step
Do not edit or optimize during the mapping session. The goal is an accurate picture of the current state, including its inefficiencies and inconsistencies.
Common discoveries at this stage include steps that different staff perform differently, steps that have no clear owner, and handoffs where information routinely gets lost.
When the session is complete, you should have a sequential list of every step from first patient contact to the defined end of the journey, with the four fields above filled in for each.
3. Gather Data and Feedback
The journey map produced in Step 2 reflects your team’s perception of the current state. Step 3 confirms which pain points are real, how frequently they occur, and how much they cost — using evidence rather than assumption.
Where to look:
Operational Data: Pull your no show rate for new patients specifically, not overall. Pull the average check in time. Pull the percentage of new patient charts that are complete when the provider enters the room.
Pull how many inbound calls per day relate to directions, parking, preparation questions, or form completion. These calls represent instructions that your process failed to deliver proactively.
Patient Feedback: Read your last 50 patient reviews and sort the comments by journey stage: booking, pre-visit, in-visit, and post-visit.
Look for language that describes friction, such as “I had to fill out the same forms twice,” “nobody told me I needed to fast,” or “I waited 40 minutes with no update.” These are not opinions. They are reports of specific process failures.
Staff input: Ask your front desk and clinical staff one question directly: “What is the one part of new patient intake that takes the most time and could be avoided?” Staff who perform the process every day know where it breaks. Their answers often point to the same two or three steps, and those steps become your confirmed priority list.
By the end of this step, you should have a shortlist of three to five specific pain points with supporting evidence, not a general sense that onboarding could be better.
Instead, you should have a concrete statement such as: “Forms are incomplete at check in for approximately 40 percent of new patients, adding an average of 12 minutes to check in and delaying clinical staff.”
4. Redesign the Journey
With confirmed pain points in hand, redesign the journey steps that cause them. This is a process design exercise, not a technology selection exercise. Start with what the process should do, then determine how to execute it.
For each confirmed pain point, work through three questions:
What outcome does this step need to produce? Be specific. “Forms complete before the patient arrives” is an outcome. “Send patients a form” is an activity. Design for the outcome.
What is preventing that outcome currently? This is usually one of four things: the patient doesn’t know the action is required, the process asks for the action too late, completing the action is harder than it needs to be, or there is no follow-up when the action isn’t completed. Identify which one applies.
What is the simplest change that addresses that cause? Resist the instinct to redesign everything at once. A single, specific change to one step is testable.
Examples include sending the intake form immediately after booking instead of at the 48 hour mark, adding one scripted follow up call for incomplete forms, or creating one standardized preparation document for each appointment type. A complete workflow overhaul is not testable.
Document the redesigned steps in the same format as your journey map: what happens, what the patient experiences, how long it takes, and what the failure modes are. The redesign should be specific enough that any staff member could follow it without additional explanation.
5. Pilot the Changes
Before applying redesigned steps across your full patient volume, test them with a defined subset. A pilot reduces risk, surfaces implementation problems before they affect every patient, and produces the early data you need to confirm the changes work.
How to structure a pilot:
Define the scope precisely. A useful pilot would be: “All new patient appointments booked in the next three weeks at one location, handled by one front desk staff member following the new intake protocol.” A poorly defined pilot such as “we will try the new approach for a while and see what happens” produces no useful data.
Brief everyone involved before the pilot starts. Staff following a new process need to understand not just what to do but why each change was made. When staff understand the reasoning, they implement more consistently and surface problems more accurately.
Run the pilot for a sufficient period. For most practices, three weeks of new patient appointments provides enough observations to identify whether the changes hold under normal volume. Fewer than two weeks rarely produces conclusive results.
Track the same metrics you identified in Step 3 throughout the pilot. If incomplete forms at check-in were the problem, count them daily during the pilot. If check-in delay was the problem, time it for each new patient. You need before-and-after numbers, not impressions.
6. Monitor and Refine
At the end of the pilot period, review the data against your baseline from Step 3. For each pain point you targeted, ask whether the metric improved, stayed the same, or got worse.
If the metric improved: Confirm that the change is the likely cause — that nothing else changed during the pilot period that could explain the result. If the improvement holds, the change is a candidate for standardization.
If the metric did not improve: Do not assume the approach was wrong before investigating why. Common reasons a pilot fails to produce improvement include inconsistent implementation, where some staff followed the new process while others reverted, or an incomplete fix that addressed only part of the root cause.
Sometimes the problem is located at a different step than the one you redesigned. Interview the staff involved, review specific cases where the pain point still occurred, and adjust the process accordingly.
Refinement at this stage is expected and normal. A process change that works perfectly on the first attempt is the exception. Plan for at least one revision cycle before moving to standardization.
7. Standardize and Scale
Once a refined change produces consistent improvement during the pilot, document it as the standard process for that journey step. Documentation must be specific enough to produce consistent behavior from any staff member who reads it. Instead of a paragraph of general principles, provide a step by step description of exactly what to do, when to do it, and how to do it.
What standardization requires:
Standardization requires a few clear elements. Each changed step should have a written protocol stored where staff can easily reference it. Provide a brief training session, not a lengthy program, just a structured walkthrough for all staff who perform that step, including new hires in the future.
Assign a defined owner for each step so one role or one person is responsible for ensuring it happens consistently. Also schedule a regular review point, typically quarterly during the first year, where metrics are checked and the protocol is updated if the process has drifted.
Once the first journey is standardized, apply the same method to the next priority journey. The process includes choosing the journey, mapping it, validating the issues, redesigning the step, running a pilot, refining the approach, and then standardizing it.
Each cycle becomes faster because the method becomes familiar. Over time, the practice builds a set of well documented and consistently executed journeys that improve the patient experience across every touchpoint.
Metrics and Ongoing Improvement
Patient journey optimization is not a one-time project. It requires continuous monitoring and iteration.
Key KPIs to track include:
- Time to next available appointment
- Online booking percentage
- Patient wait times
- No-show and cancellation rates
- Call volume and call resolution
- Patient satisfaction and loyalty
- Retention and repeat visits
Set baselines, define realistic targets, and review metrics regularly with the care team. Combine quantitative data with qualitative feedback from patients and staff to run small experiments and refine the journey design.
Conclusion
Patient journey optimization helps healthcare organizations move from fragmented interactions to a clear, connected end-to-end patient journey. By mapping journey stages, improving touchpoints, leveraging digital tools, and measuring performance, clinics can reduce friction, improve outcomes, and create better patient experiences.
A practical place to start is simple: choose one patient journey, map it with your team, identify three pain points, and design one small improvement for each. Over time, these changes add up to better care, happier patients, and more efficient operations.
FAQs
What are the main stages of a typical patient journey?
A typical patient journey includes awareness, research, appointment booking, pre-visit preparation, in-visit care, and post-visit follow-up.
What are common pain points in the patient journey?
Common pain points include difficult booking, long wait times, unclear instructions, poor communication, and confusing billing.
Can smaller clinics or practices benefit from patient journey optimization?
Yes. Smaller clinics often see faster improvements because fewer systems and teams make changes easier to implement.
How often should patient journey maps be updated?
Journey maps should be reviewed at least annually or whenever there are major process, technology, or service changes.
How do we collect useful patient feedback for journey optimization?
Use short surveys, follow-up messages, reviews, and direct patient conversations at key journey touchpoints.